For new nurses and midwives, resilience is essential for navigating the steep learning curve, and emotional challenges of transitioning from student to professional. This nonexperimental, descriptive study aimed to evaluate the resilience levels of newly qualified nurses and midwives in Western Australia (WA) who completed new graduate programs during 2021/2022. We sought to understand how graduates adapted to the challenges of clinical practice, at the time of the COVID-19 pandemic. A survey design was employed, targeting WA nurses and midwives who participated in structured new graduate programs. Participants were recruited via the WA Department of Health GradConnect system and completed an online survey, which included demographic questions and the 25-item Connor-Davidson Resilience Scale (CD-RISC). Data were analysed using RStudio to determine resilience scores and key contributing factors. Out of 400 invited participants, 88 responded (22%), with 75 completing the full survey (19% completion rate). The mean resilience score was 74.9 (SD = 9.1), placing most graduates in the lower to moderate quartiles of the general population. Key strengths included self-efficacy and adaptability, while lower scores were observed in emotional regulation, optimism, spiritual coping, and leadership confidence. WA graduate nurses and midwives showed promising levels of resilience amid significant workforce shortages and pandemic pressures. The findings affirm that resilience-building is not optional but essential for workforce sustainability, reinforcing the need for strategies that strengthen coping capacity and retention during times of crisis and beyond.
Key Words: Resilience, graduates, nurses, midwives, workforce issues, structured graduate programs, retention, adaption
Western Australia (WA), the largest state in Australia, covers approximately 33% of the country's total land area but remains sparsely populated, with only 10.9% of the national population (Government of WA, 2024). While most residents are concentrated in the metropolitan area, a modest amount live in regional and remote areas characterised by low population densities and vast distances between communities (Regional Studies Association, 2025). Recent data indicates that WA has the lowest nurse-to-population ratio of all Australian states, which exacerbates the challenge between access, quality and cost of healthcare (Australian Institute of Health and Welfare [AIHW], 2024). Other factors include shortages of healthcare professionals, ageing populations with an increased demand for care, the growing burden of chronic and complex conditions, the cost of treatment and technology, and heightened consumer expectations (AIHW, 2024).
While the global nursing shortage is well-documented, the situation regarding new graduate nurses is complex. In some regions, there appears to be an oversupply of new graduates, leading to challenges in securing employment (Doleman et al., 2024). However, this perceived oversupply does not necessarily contradict the overall shortage where factors such as high turnover rates among novice nurses contribute to this paradox. Additionally, rural regions continue to face significant shortages, further exacerbated by low numbers of new graduate nurses (Australian Government, Department of Health & Aged Care, 2024). Moreover, the reluctance of some healthcare facilities to hire inexperienced nurses without sufficient support structures further complicates the employment landscape for novice graduates (Church, 2024).
The first year of employment for the novice nurse or midwife often occurs through a graduate program. In WA, new graduate nurses and midwives transition into clinical practice through structured programs designed to support their development and integration into the healthcare workforce (Rogers et al., 2023). Programs offer hands-on experience in various clinical settings, allow graduates to consolidate their theoretical learning, and develop critical clinical skills and judgment (Government of WA, Department of Health, 2025; Masso et al., 2022). The first 12-24 months of time in a professional nursing or midwifery role is essential to success and tenure in the role, and also the time for the consolidation of competence and confidence in the workplace (Charette et al., 2023). New graduate programs enhance practice readiness by fostering resilience and professional identity through structured clinical experience (Rogers et al., 2023) and social integration (Baharum et al., 2023).
For new nurses and midwives, resilience—the ability to adapt, cope, and grow in the demanding and often stressful healthcare environment—is essential for navigating the steep learning curve, and emotional challenges of transitioning from student to professional (Smythe & Carter, 2022). This transition is often marked by “reality shock” (Kramer, 1974) and vulnerability as described in Duchscher’s transition theory (2008, 2009), which emphasises the challenges and emotional, cognitive, and social adjustments required to bridge the gap between expectations and reality during the first year of practice.
Resilience is critical not only for individual wellbeing and job satisfaction but also for workforce sustainability, as new graduates face high stress conditions, such as managing shift work, increased patient acuity, technological changes, and staff shortages, all while developing trust in their professional judgment (Randall et al., 2023). Unexpected local or global events (e.g., the COVID-19 pandemic) further amplify these challenges. Factors that influence resilience include self-efficacy, adaptability, coping strategies such as humour and spirituality, and the ability to manage uncertainty and ethical decision-making (Yilmaz, 2017). Understanding these factors is vital for designing interventions that reduce burnout, strengthen coping mechanisms, and improve retention (Mealer, 2020). Thus, resilience is fundamental to ensure wellbeing and to strengthen the nursing and midwifery workforce in contemporary healthcare settings.
During the COVID-19 pandemic in WA, newly qualified nurses and midwives faced considerable challenges as they entered the workforce. Despite strict containment measures, including a hard border closure (April 2020 to February 2022), hotel quarantine and regional lockdowns, the pandemic exacerbated existing staffing shortages. Graduates faced heavier workloads, frequent overtime, and reduced access to support systems, while managing the constant fear of infection, the risk of exposing loved ones (Doleman et al., 2024), and the need to adapt to constantly evolving infection control protocols (Dann & Sun, 2022). These conditions created a high-stress environment that tested resilience and coping strategies, which required rapid adaption to a system facing unprecedented challenges. Understanding how resilience functions under such circumstances is critical to inform graduate support programs and mitigate transition shock.
Workforce shortages and the challenges of transitioning into professional practice have long affected the healthcare sector, but their impact has intensified in recent years. These persistent pressures threaten workforce sustainability and heighten the vulnerability of graduates during their critical first year. Resilience is a key protective factor in this context, enabling graduates to adapt, cope, and remain in the profession despite systemic strain. This study examined the resilience levels of nurses and midwives who completed new graduate programs in Western Australia in 2021/2022, providing insights to inform strategies that strengthen graduate support and retention.
Methods
Design
This study used a nonexperimental, descriptive survey research design to evaluate the reported resilience of nurses and midwives in a program for nurses who had just graduated their initial program. (AUTHORS: I changed the wording of this a little bit because the words “graduate program” in a US journal typically mean a program for graduate education resulting in a masters or higher degree and thus readers are likely to misunderstand this as nurses in graduate school. You do give additional context about this pretty regularly throughout the article, but I think we need to do that as often as possible as we can. I am hoping this language will work for you but if not let me know and we will talk about it until we can reach consensus. Jackie) The aim was to evaluate newly qualified nurses and midwives’ levels of resilience during their graduate year. The study was guided by the Australian Code for Responsible Conduct of Research (Australian Government, 2018) and received ethical approval from The University of Notre Dame (Australia) Human Research Ethics Committee.
Population
The population of interest was WA registered nurses, enrolled nurses and midwives who commenced a new graduate program at their place of employment in 2021 and completed in 2021/2022 (n=400). A Registered Nurse is a degree-qualified professional licensed by a national regulatory authority to provide clinical care, make decisions, supervise staff, and collaborate with interprofessional teams (Nursing and Midwifery Board, 2025). In Australia and New Zealand, an Enrolled Nurse holds a diploma and works under the supervision of a Registered Nurse. Equivalent roles internationally include Nursing Associate in the UK and Licensed Practical Nurse (LPN) in the United States (U.S) and Canada. Inclusion criteria were registered/enrolled nurses or midwives employed in a formal structured transition to practice program in participant WA public, private and aged care health providers. An exclusion criterion was any nurse or midwife employed as a first-year level 1 without a formal graduate program. Participants were recruited through the WA Department of Health GradConnect online system (Government of WA Department of Health, 2025).
Data Collection
Participants were invited to participate via an email containing the participant information sheet and a link to the survey from May 2021 to February 2022. Email addresses were provided by the GradConnect system (Government of WA Department of Health, 2025). An online survey (Qualtrics, 2022) was used and included a consent question in the first section of the survey, demographic information questions, and the Connor-Davidson Resilience Scale ([CD-RISC]; Connor & Davidson, 2003). The survey comprised a total of 33 questions, including consent = 1, demographics = 7, and Connor-Davidson Resilience Scale = 25). Please see the supplemental material link here for the demographic survey questions and the CD-RISC.
Demographic Information
Demographic information collected through the online survey included: age (18-27, 28-37, 38-47 and 48+), sex (male, female, other, prefer not to say), aboriginal descent (yes/no), current registration (registered nurse, enrolled nurse, registered midwife), and program speciality (General Surgery, Mental Health, Paediatrics, Critical Care, General Medicine, Midwifery, Perioperative, Other). All questions used multiple-choice formats to enhance ease of completion and improve response rates.
Connor-Davidson Resilience Scale
The Connor-Davidson Resilience Scale ([CD-RISC]; 2003) is a psychological assessment tool developed to measure resilience (positive adaption in response to stress, adversity, or trauma) in both general and clinical populations. The CD-RISC consists of 25 items that assess overall resilience levels while also evaluating key subscales such as hardiness (7 items), coping ability (5 items), adaptability/flexibility (3 items), sense of meaning and purpose (4 items), optimism (2 items), emotional and cognitive regulation (2 items), and self-efficacy (2 items). The tool uses a five-point Likert scale scored from 0 to 4 (0-not true at all, 1-rarely true, 2-sometimes true, 3-often true, and 4-true nearly all the time). A higher score reflects greater resilience, while lower scores indicate reduced resilience.
The CD-RISC 25 demonstrates strong reliability in general populations, with a Cronbach’s alpha of 0.89, indicating high internal consistency. Test-retest reliability is also strong (ICC = 0.87), showing stability over time (Connor & Davidson, 2003). Based on the Connor and Davidson (2003) recommendations, the scale was measured using Quartiles based on general population scores (i.e., Q1, Q2, Q3, Q4). Q1 contains scores from 0-73 and reflects the least resilient 25% of the general population, Q2 contains scores between 74-82, Q3 contains scores between 83-90 and Q4 contains scores from 91-100 and reflects the most resilient 25% of the population
Data Analysis
Data was analysed in RStudio version 4.5.1 (Posit Software, 2024) and were summarised using mean (SD), minimum and maximum for continuous variables and count and frequency percentages for categorical variables. Resilience as scored by the CD-RISC is the primary outcome.
Results
The survey was distributed to 400 WA nurses and midwives. 88 participants (22%) consented and completed demographic information, however only 75 completed all questions (19% response rate).
Demographic Data
Most participants were female (92%, 81/88) and selected the age range 18 to 27 years old (58%, 52/88). Majority were registered nurses (75%, 66/88) and enrolled nurses (16%, 14/88). All demographic data is displayed in Table 1.
Table 1. Demographic Information
|
Characteristic |
|
|---|---|
|
Sex, n (%) |
|
|
Female |
81 (92%) |
|
Male |
6 (7%) |
|
Age, n (%) |
|
|
18-27 years of age |
52 (59%) |
|
28-37 years of age |
16 (18%) |
|
38-47 years of age |
14 (16%) |
|
48+ years of age |
6 (7%) |
|
Descent, n (%) |
|
|
Aboriginal descent |
3 (3%) |
|
Aboriginal and Torre Strait Islander descent |
1 (1%) |
|
Current nursing registration, n (%) |
|
|
Registered nurse |
66 (75%) |
|
Enrolled nurse |
14 (16%) |
|
Registered nurse and midwife |
7 (8%) |
|
Registered nurse and enrolled nurse |
1 (1%) |
|
Registered midwife* |
0 (0%) |
Note. * Enrolled nurse is equivalent to a Nursing Associate/Licensed Practical Nurse **In WA midwifery is mainly a postgraduate course of study
Resilience: CD-RISC
The mean (SD) resilience score for the participants was 74.9 (9.1) with a median score of 74. The minimum score recorded was 45 and the maximum 93. Of the participants, 45% (n=34) scored in the lowest quartile Q1 (score range 0-73, median 70.5 mean 69.1 and SD 3.3) of the general population and have low resilience. 35% (n=26) and 13% (n=10) of participants scored in Q2 (score range 74-82, median 77, mean 77.5, SD 2.7) and Q3 (score range 83-90, median 85, mean 86, SD 39.7) of the general population, representing moderate resilience. 7% (n=5) scored in the highest quartile Q4 (score range 91-100, median 92, mean 92, SD 1.0) of the general population and have high resilience.
Resilience: Key Factors
The CD-RISC-25 examines participants key factors of resilience: hardiness, coping, adaptability/flexibility, meaningfulness/purpose, optimism, regulation of emotion and cognition, and self-efficacy. The participant results are displayed graphically in Figure 1 below.
Figure 1. Key Factors of Resilience as Scored by Connor-Davidson Resilience Scale
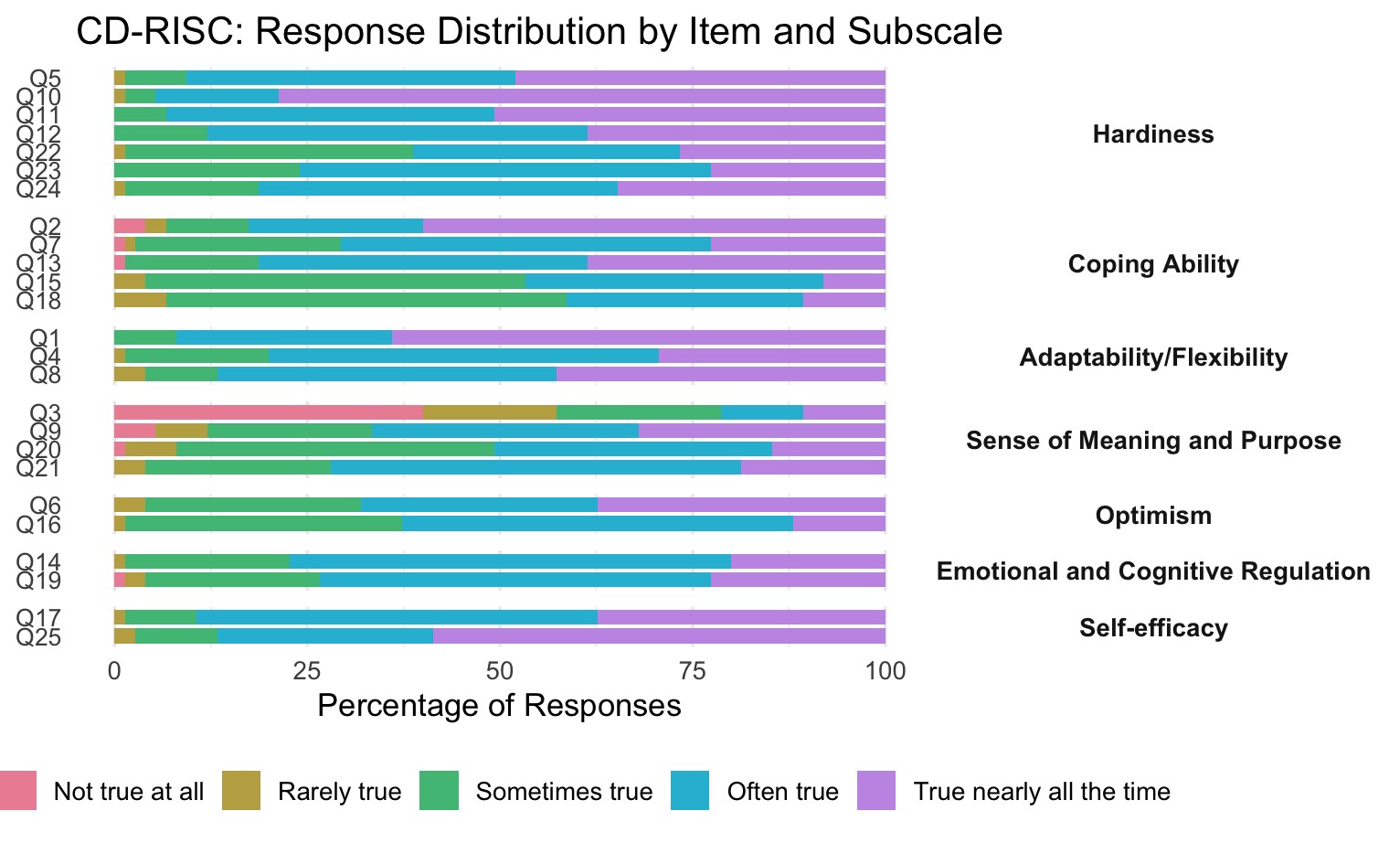
Discussion
Resilience is a critical protective factor for new graduates navigating the transition from education to professional practice, particularly in high-pressure contexts such as workforce shortages and unexpected events like the COVID-19 pandemic. This study’s findings indicated that graduates who completed programs in WA during 2021/2022 demonstrated moderate to high levels of resilience, an outcome that was somewhat unexpected given the compounded stressors of staffing deficits, increased workloads, and systemic strain. These results suggested that while the transition period remains challenging, resilience among this cohort was sufficiently developed to support adaptation and coping, which aligns with the theoretical premise that resilience mitigates transition shock (Duchscher, 2008; Kramer, 1974).
In this study, new graduates demonstrated resilience levels comparable to or higher than similar nursing cohorts (Al Hadid et al., 2021; Chesak et al., 2015; Harmon, 2023; Irwin et al., 2021; Zhang et al., 2024), and an Australian community sample aged 28–32 (mean 71.5) (Liu et al., 2015). These findings indicated resilience is present but still developing under demanding conditions. Scores were lower than the general U.S. adult average (mean 79) reported in CD-RISC 25 guidelines (Connor & Davidson, 2020) which suggested that graduates encounter complex situations that can create uncertainty (Alharbi et al., 2023) and which may diminish their perceived resilience. Although determination and adaptability were evident, these qualities were tested by the unprecedented pressures of the clinical environment during the pandemic (Doleman et al., 2024). New graduates’ ability to manage unpredictability is emerging, yet their sense of control may fluctuate as experience grows. This pattern is supported by Prosen and Ličen (2023) who noted that despite daunting post-pandemic demands, graduates adapted quickly and demonstrated commitment and responsibility in their new roles.
Self-efficacy emerged as a major strength, which reflects graduates’ confidence in their ability to manage challenges. Cheraghi et al. (2009) identified this belief as critical for successful adaptation, and Wang et al. (2018) confirmed its role in supporting resilience among novice nurses. Adaptability and flexibility were also evident, which indicates graduates could adjust to changing circumstances. Baharum et al. (2023) further noted that proactivity—taking initiative to prevent future issues—contributes significantly to resilience in this cohort. High self-efficacy allows novices to build on early successes, which fosters confidence and strengthens resilience during the transition to practice. Similarly, Labrague and McEnroe-Petitte’s (2018) review found that despite workplace challenges, new graduates persisted and adapted to the fast-paced, unpredictable nature of healthcare. Thus, their willingness to adapt supported integration into interprofessional teams and engagement with diverse patient populations (Baharum et al., 2023).
Mid-range CD-RISC scores suggested that resilience traits are present but not consistently strong. These responses indicate developing or situationally activated behaviours, such as a reasonable belief in managing adversity, the ability to stay composed under pressure, and the capacity to recover quickly after hardship. Curiosity and openness to challenges point to potential for growth, yet anxiety and self-doubt remain common in early practice (Prosen & Ličen, 2023). Graduates value learning opportunities but may find them intimidating. Composure and decision-making are still developing, while stress can compromise focus during critical moments. However, this is a normal aspect of building clinical judgment under pressure (Sherman, 2021). Overall, these moderate scores reflected a functional level of resilience, with emerging strengths in help-seeking, coping, and recovery. This foundation can be reinforced through supportive environments, mentoring, reflective practice, and workload management.
Resilience is multifaceted and shaped by personal and systemic factors. Lower scores in optimism, spiritual coping, and leadership highlight areas that require targeted support during transition. These traits reflect common vulnerabilities among new graduates. Limited reliance on spiritual framing for coping may mirror broader societal trends, particularly in Western contexts where religious affiliation and participation has declined. Emotional regulation strategies such as spiritual reframing or humour appear underdeveloped in the first year and are not consistently relied on during stress. Spirituality can help restore emotional balance, reduce anxiety and depression, and enhance resilience and career satisfaction (Pinnex, 2024). Likewise, humour offers perspective in tense situations, creating distance and a reduction in perceived stress (Canestrari et al., 2021). Therefore, strengthening these strategies could provide graduates with additional tools to manage pressure and maintain wellbeing.
Kramer’s (1974) concept of reality shock and Duchscher’s (2008, 2009) transition theory frame the vulnerability of new graduates, and the findings align with these perspectives. While resilience supports adaptation, confidence and coping remain fragile in early months of practice. Independence and assertiveness are still forming but often constrained by limited clinical experience (Alharbi et al., 2023; Lee & Sim, 2020) and hierarchical structures within healthcare (Baharum et al., 2023). Novices tend to rely on structured knowledge and guidelines rather than intuitive reasoning (Masso et al., 2022), which typically develops through repeated exposure to similar cases, a process new graduates have not yet experienced (Corick et al., 2024). Uncertainty around professional boundaries may also limit initiative, particularly in multidisciplinary teams or under senior supervision. This can lead to hesitation during conflict or decision-making, often driven by fear of mistakes (Willman et al., 2021).
Leadership emerged as another area of vulnerability, with graduates reporting stress when required to make decisions affecting others. Problem-solving determination is developing but may falter in ambiguous or complex scenarios, prompting novices to seek reassurance rather than act independently (Najafi & Nasiri, 2023). Consequently, criticism may be internalised, leading to self-doubt or emotional withdrawal (Yang et al., 2025). Hence, resilience in the face of failure remains tenuous and strongly influenced by workplace culture and how mistakes are managed. This underscores the need to foster courageous leadership which promotes speaking up for safety, accountability, and empowerment of others (Tye et al., 2022), and to build ethical confidence, which reflects assurance in ethical knowledge and decision-making capacity to advocate for patients and maintain integrity (Pajakoski et al., 2021) during the graduate period.
A supportive environment is essential for work readiness, enabling graduates to progress from partial responsibility during orientation to full responsibility within weeks of commencing a program (Graf et al., 2020; Rogers et al., 2023). Such support protects and sustains the nursing profession during times of challenge. Low resilience may reflect individual traits or systemic issues, which highlights the need for targeted strategies that build decision-making confidence, strengthen coping with uncertainty, and reduce anxiety. Chesak (2015) demonstrated the effectiveness of stress management and resiliency training, with mindfulness reducing stress and increasing resilience scores. For contemporary graduate programs, resilience-building is not optional but fundamental. While this cannot eliminate workplace stress, it equips graduates to manage adversity and maintain performance under pressure (Harmon, 2023; Cao et al., 2021).
In summary, the findings from this study underscore resilience as foundational for the nursing and midwifery workforce. Despite the unprecedented pressures from ongoing systemic challenges, graduates demonstrated resilience levels comparable to or exceeding similar populations, which acknowledges the value of structured graduate programs in the promotion of adaptability and self-efficacy. However, lower scores in optimism, spiritual coping, and leadership reveal areas for targeted support. The findings affirm that resilience-building is not optional but essential for workforce sustainability, reinforcing the need for strategies that strengthen coping capacity and retention during times of crisis and beyond.
Limitations
This study had several limitations. The data, collected during 2021–2022, reflect the context of the COVID-19 pandemic and may not fully capture more recent shifts in the healthcare workforce, including post-pandemic recovery, climate-related disruptions, ongoing staffing shortages, and workforce safety concerns. Although the study was conducted in WA and may not be fully generalisable to other settings, the findings may still be relevant to regions with similar healthcare challenges, such as Queensland, the Northern Territory, and parts of Canada, the United States, and New Zealand. The 19% response rate, though within acceptable ranges for healthcare research, highlights persistent barriers to participation, including workforce fatigue, psychological strain, and survey saturation. Additionally, the study relied solely on quantitative data; qualitative methods such as interviews or focus groups could have provided deeper insight into lower-scoring areas like leadership and initiative.
Implications for Practice
The findings of this study have practical implications beyond the WA context. Core resilience traits such as adaptability and self-efficacy are likely to be relevant to newly qualified nurses and midwives in other settings who face similar workforce pressures. However, resilience is multidimensional, and strategies should also consider factors such as workplace culture, opportunities for social integration, and personal coping mechanisms, including spirituality and humour. Structured graduate programs, mentoring, and targeted support strategies can be adapted to suit diverse healthcare environments. With the implementation of interventions that foster resilience, healthcare organisations can enhance workforce retention, reduce burnout, and support the transition of new graduates into clinical practice. While contextual differences exist, insights from the study may contribute to a broader understanding of how to support early-career health professionals in contemporary healthcare landscapes.
Conclusions
Resilience in new graduates is essential to manage the high stress, emotional demands, and rapidly increasing responsibilities in today’s complex healthcare environment. This evaluation highlights the need to actively build resilience so novices can adapt to the pressures of clinical practice and manage patient and staff challenges effectively. Strengthening resilience also supports emotional and behavioural regulation during unexpected local and global events and helps maintain well-being. To promote the retention of nurses and midwives from the early career stage, and their transition from novice to proficient, good coping abilities, healthy support seeking behaviours and structured support programs are critical. When combined with positive workplace cultures and targeted early interventions, these strategies can enhance graduates’ professional growth, leadership potential, and long-term sustainability in the workforce.
Authors
Tracey H. Coventry, PhD, MNurseEd, BSN, RN
Email: Tracey.coventry@nd.edu.au
ORCID ID: 0000-0003-3228-6448
Tracey Coventry is an experienced health professional, researcher, and senior policy leader in the private health sector, and currently serves on the board of Sheridan Institute of Higher Education. She holds a PhD in education and leadership, with a clinical background in nursing and midwifery, having trained at the Royal Children’s Hospital in Melbourne and in Scotland respectively. Tracey has held senior academic roles at The University of Notre Dame Australia, including Program Coordinator for Health Leadership and Education and Postgraduate Coordinator in the School of Nursing and Midwifery. Her career includes extensive experience in clinical leadership, healthcare policy development, and paediatric and general acute care education. She continues to contribute actively to research, policy, and governance in health and education.
Molly Coventry, BPhysio (Hons)
Email: m.coventry@edu.edu.au
ORCID ID: 0009-0009-4066-5262
Molly Coventry is a physiotherapist with a strong focus on musculoskeletal and sports injury management. She holds a Bachelor of Physiotherapy with First Class Honours and is currently pursuing a PhD, conducting novel research in muscle and tendon injuries. Molly is experienced in patient assessment, manual therapy, and evidence-based rehabilitation, with a commitment to long-term recovery and performance outcomes. She is known for her clear communication, collaborative approach within multidisciplinary teams, and dedication to patient-centred care. In addition to her doctoral studies, she works part-time as a research assistant, contributing to ongoing clinical research projects.
Kylie P. Russell, PhD, MHSE, BSN, RN
Email: Kylie.russell@nd.edu.au
ORCID ID: 0000-0001-9737-8533
Professor Kylie Russell holds a PhD in Education and a Master of Health Science, with extensive experience across both healthcare and higher education sectors. She currently serves as Head of Quality, Assessment, and Medicines Associated Programs in the School of Medicine at The University of Notre Dame, Australia. Her previous academic roles include Associate Dean and Postgraduate Coordinator in the School of Nursing and Midwifery. In the WA Health system, Kylie has held diverse leadership and clinical roles including Clinical Nurse Manager, Clinical Nurse Consultant, Staff Educator, HR Manager, and Project Officer. Her work focuses on advancing education quality, supporting research initiatives, and fostering a culture of scholarship in health professional programs.
References
Al Hadid, L. A. E., Al Barmawi, M. A., Alnjadat, R., & Farajat, L. A. (2022). The impact of stress associated with caring for patients with COVID-19 on career decisions, resilience, and perceived self-efficacy in newly hired nurses in Jordan: A cross-sectional study. Health Science Reports, 5(6), e899. https://doi.org/10.1002/hsr2.899
Alharbi, H. F., Alzahrani, J., Hamed, A., Althagafi, A., & Alkarani, A.S. (2023). The experiences of newly graduated nurses during their first year of practice. Healthcare (Basel), 11(14), 2048. https://doi.org/10.3390/healthcare11142048
Australian Government. (2018). Australian code for the responsible conduct of research 2018. National Health and Medical Research Council, Australian Research Council and Universities Australia. https://www.nhmrc.gov.au/about-us/publications/australian-code-responsible-conduct-research-2018
Australian Government, Department of Health and Aged Care. (2024). Nurse supply and demand study 2023–2035. https://hwd.health.gov.au/resources/primary/nursing-supply-and-demand-study-2023-2035.pdf
Australian Institute of Health and Welfare. (2024). Health workforce. https://www.aihw.gov.au/reports/workforce/health-workforce
Baharum, H., Ismail, A., McKenna, L., Mohamed, Z., Ibrahim, R., & Hassan, N. H. (2023). Success factors in adaptation of newly graduated nurses: A scoping review. BMC Nursing, 22(1), Article 125. https://doi.org/10.1186/s12912-023-01300-1
Canestrari, C., Bongelli, R., Fermani, A., Riccioni, I., Bertolazzi, A., Muzi, M., & Burro, R. (2021). Coronavirus disease stress among Italian healthcare workers: The role of coping humor. Frontiers in Psychology, 11, 601574. https://doi.org/10.3389/fpsyg.2020.601574
Cao, X., Li, J., & Gong, S. (2021). The relationships of both transition shock, empathy, resilience and coping strategies with professional quality of life in newly graduated nurses. BMC Nursing, 20(1), 65. https://doi.org/10.1186/s12912-021-00589-0
Charette, M., McKenna, L. G., Deschênes, M.-F., Ha, L., Merisier, S., & Lavoie, P. (2023). New graduate nurses’ clinical competence: A mixed methods systematic review. Journal of Advanced Nursing, 76(11), 2810–2829. https://doi.org/10.1111/jan.14487
Cheraghi, F., Hassani, P., Yaghmaei, F., & Alavi-Majed, H. (2009). Developing a valid and reliable self-efficacy in clinical performance scale. International Nursing Review, 56(2), 214–221. https://doi.org/10.1111/j.1466-7657.2008.00685.x
Chesak, S. S., Bhagra, A., Schroeder, D. R., Foy, D. A., Cutshall, S. M., & Sood, A. (2015). Enhancing resilience among new nurses: Feasibility and efficacy of a pilot intervention. The Ochsner Journal, 15(1), 38–44. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4365845/
Church, E. (2024). New nurses struggle to find jobs despite national shortage. Nursing Times. https://www.nursingtimes.net/education-and-training/new-nurses-struggle-to-find-jobs-despite-national-shortage-20-06-2024/
Connor, K. M., & Davidson, J. R. T. (2003). Development of a new resilience scale: The Connor-Davidson Resilience Scale (CD-RISC). Depression and Anxiety, 18(2), 76–82. https://doi.org/10.1002/da.10113
Connor, K. M., & Davidson, J. R. T. (2020). Scoring and interpretation of the Connor-Davidson Resilience Scale (CD-RISC) [Unpublished manuscript].
Corick, H., Clarke, B., & Ikenna-Ezekiel, J. (2024). The role of intuition in nurse decision making. BJN Inform. https://www.bjninform.com/my-career/the-role-of-intuition-in-nurse-decision-making/
Dann, C., & Sun, Z. (2022). The impact of COVID-19 on Western Australian medical imaging clinical practice and workplace. Journal of Medical Radiation Sciences, 69(3), 299–308. https://doi.org/10.1002/jmrs.594
Doleman, G., Leo, A. D., & Bloxsome, D. (2024). The impact of the COVID-19 pandemic on nurses’ and junior doctors’ workloads. Journal of Advanced Nursing, 81(7), 3729–3738. https://doi.org/10.1111/jan.16487
Duchscher, J. E. B. (2008). A process of becoming: The stages of new nursing graduate professional role transition. The Journal of Continuing Education in Nursing, 39(10), 441–450. https://doi.org/10.3928/00220124-20081001-03
Duchscher, J. E. B. (2009). Transition shock: The initial stage of role adaptation for newly graduated registered nurses. Journal of Advanced Nursing, 65(5), 1103–1113. https://doi.org/10.1111/j.1365-2648.2008.04898.x
Graf, A., Jacob, E., Twigg, D., & Nattabi, B. (2020). Contemporary nursing graduates’ transition to practice: A critical review of transition models. Journal of Clinical Nursing, 29(15–16), 3097–3107. https://doi.org/10.1111/jocn.15234
Government of Western Australia. (2024). Population. https://www.wa.gov.au/organisation/department-of-treasury/population
Government of Western Australia, Department of Health. (2025). 2025 GradConnect. https://www.health.wa.gov.au/GradConnect
Harmon, R. G. (2023). Building resilience in graduate nurses through online virtual simulation (Doctoral dissertation). Abilene Christian University. https://digitalcommons.acu.edu/cgi/viewcontent.cgi?article=1571&context=etd
Irwin, K. M., Saathoff, A., Janz, D. A., & Long, C. (2021). Resiliency program for new graduate nurses. Journal for Nurses in Professional Development, 37(1), 35–39. https://doi.org/10.1097/NND.0000000000000678
Kramer, M. (1974). Reality shock: Why nurses leave nursing. Mosby.
Labrague, L. J., & McEnroe-Petitte, D. M. (2018). Job stress in new nurses during the transition period: An integrated review. International Nursing Review, 65(4), 491–504. https://doi.org/10.1111/inr.12425
Lee, J. E., & Sim, I. O. (2020). Gap between college education and clinical practice: Experience of newly graduated nurses. Nursing Open, 7, 449–456. https://doi.org/10.1002/nop2.409
Liu, D. W. Y., Fairweather-Schmidt, A. K., Burns, R. A., & Roberts, R. M. (2015). The Connor-Davidson Resilience Scale: Establishing Invariance Between Gender Across the Lifespan in a Large Community Based Study. Journal of Psychopathology and Behavioral Assessment, 37(2), 340–348. https://doi.org/10.1007/s10862-014-9452-z
Masso, M., Sim, J., Halcomb, E., & Thompson, C. (2022). Practice readiness of new graduate nurses and factors influencing practice readiness: A scoping review of reviews. International Journal of Nursing Studies, 129, Article 104208. https://doi.org/10.1016/j.ijnurstu.2022.104208
Mealer, M. (2020). Coping with caring: A nurse’s guide to better health and job satisfaction (1st ed.). Routledge.
Najafi, B., & Nasiri, A. (2023). Explaining novice nurses’ experience of weak professional confidence: A qualitative study. SAGE Open Nursing, 9, 23779608231153457. https://doi.org/10.1177/23779608231153457
Nursing and Midwifery Board. (2025). Registration and endorsement. https://www.nursingmidwiferyboard.gov.au/registration-and-endorsement
Pajakoski, E., Rannikko, S., Leino-Kilpi, H., & Numminen, O. (2021). Moral courage in nursing: An integrative literature review. Nursing & Health Sciences, 23(3), 570–585. https://doi.org/10.1111/nhs.12805
Pinnex, K. (2024). Is spirituality the key to nurses triumphing over stress? Minority Nurse. https://minoritynurse.com/is-spirituality-the-key-to-nurses-triumphing-over-stress/
Posit Software, PBC. (2024). RStudio (Version 4.5.1) [Computer software]. https://posit.co
Prosen, M., & Ličen, S. (2023). Newly graduated nurses’ perceptions of their professional role and professional competency: A qualitative focus group study. BMC Medical Education, 23(1), Article 755. https://doi.org/10.1186/s12909-023-04747-7
Qualtrics. (2022). Qualtrics software (Version March 2022). https://www.qualtrics.com
Randall, P. S., De Gagne, J. C., Lee, E., Slack, J., Lee, Y., & Ledbetter, L. (2023). The experience of resilience in newly graduated nurses: A qualitative metasynthesis. Nurse Education in Practice, 70, Article 103681. https://doi.org/10.1016/j.nepr.2023.103681
Regional Studies Association. (2025). Regional development in Australia’s biggest state: Western Australia. https://www.regionalstudies.org/rsa-blog/regional-development-in-australias-biggest-state-western-australia/
Rogers, S., Lai, J., Walker, A., Rawson, H., & Redley, B. (2023). Development of work readiness in graduate nurses during a transition to practice program: A survey study. Collegian, 30(4), 595–601. https://doi.org/10.1016/j.colegn.2023.05.007
Sherman, R. O., & Labat, A. M. (2021). Managing new nurse fear and anxiety: Simple strategies can help with transition to practice. American Nurse Journal, 16(4), 37. https://www.myamericannurse.com/wp-content/uploads/2021/02/an4-Fear-318.pdf
Smythe, A., & Carter, V. (2022). The experiences and perceptions of newly qualified nurses in the UK: An integrative literature review. Nurse Education in Practice, 62, Article 103338. https://doi.org/10.1016/j.nepr.2022.103338
Tye, J., Hanrahan, K., Edmonds, S., Hyatt, D., & Tye, A. (2022). Courageous leadership for a culture of emotional safety. Nursing Management, 53(11), 16–23. https://doi.org/10.1097/01.NUMA.0000891468.54597.90
Wang, L., Tao, H., Bowers, B. J., Brown, R., & Zhang, Y. (2018). Influence of social support and self-efficacy on resilience of early career registered nurses. Western Journal of Nursing Research, 40(5), 648–664. https://doi.org/10.1177/0193945916685712
Willman, A., Bjuresäter, K., & Nilsson, J. (2021). Insufficiently supported in handling responsibility and demands: Findings from a qualitative study of newly graduated nurses. Journal of Clinical Nursing, 30(1–2), 83–92. https://doi.org/10.1111/jocn.15483
Yang, R., Li, N., Fan, Y., Yuan, Z., Lin, C., Shen, Y., & Yang, L. (2025). The relationship between clinical nurses’ feelings of underqualification and work withdrawal behavior: The multiple mediating roles of self-disgust and self-efficacy. Frontiers in Psychology, 16, 1588917. https://doi.org/10.3389/fpsyg.2025.1588917
Yilmaz, E. B. (2017). Resilience as a strategy for struggling against challenges related to the nursing profession. Chinese Nursing Research, 4, 9-13. https://doi.org/10.1016/j.cnre.2017.03.004
Zhang, Y., Shen, M., & Huang, H. (2024). Resilience’s role in clinical belongingness and presenteeism of new nurses: A moderated mediation model. Nursing & Health Sciences, 26(1), e13078. https://doi.org/10.1111/nhs.13078

