The Food Allergy Nurses Interest Group (FANI) proposes establishing a Certified Allergy Nurse Educator (ANE) role to improve access to care and address disparities. The authors seek to understand perceptions of the ANE role and its value. An article published in Allergic Living Magazine (2022) highlighted potential benefits of the ANE for providers, patients, and caregivers. The article included a brief three-question survey and a comments section to collect informal feedback from readers. Analyzing 178 survey responses from patients, nurses, allergists, and other healthcare professionals across 36 states and three countries showed strong support for ANEs. Comments emphasized certification, training, patient advocacy, personal experiences, implementation, and general interest. This valuable feedback guides future steps in developing the ANE role and advancing allergy specialization within nursing. By optimizing resources, we can improve care delivery and outcomes, especially in preventing and managing allergies among the increasing number of affected individuals in the U.S.
Key Words: Certified Allergy Nurse Educator; ANE role; Allergy Nurses; Food Allergy Nurses Interest Group; FANI; Allergy Nursing Specialty
The prevalence of food allergies continues to increase in both pediatric and adult populations. According to the Centers for Disease Control (CDC, 2023), more than a quarter of U.S. adults and children have at least one allergy, with food allergies being more common among Black, non-Hispanic children and adults compared to Hispanic or White populations (Ng & Boersma, 2023; Zablotsky et. al, 2023). Nurses are often on the front lines of patient care and education, especially regarding chronic and acute conditions like allergies. As nurses remain highly trusted professionals (Gallup, 2024), it is our duty to ensure care that is timely, affordable, and equitable. While some individuals can easily access a primary care physician or an allergist within their health insurance plans, this is not always the case for many living in rural, underrepresented, and underserved communities across the United States. Currently, there are approximately 7,282 board-certified Allergists and Immunologists in the U.S. (American Board of Allergy and Immunology, n.d.). A recent study found that providers in rural areas were less likely to accept Medicaid compared to those in urban areas. Of 5,694 allergists surveyed, 55.5% accepted Medicaid, including providers in 13 out of 51 states and Washington, D.C., with acceptance rates ranging from 13% in New York to 90% in New Mexico (Ho et al., 2024). As the demand for specialists grows alongside the increasing prevalence of allergies, and given the shortage of qualified providers—especially outside urban centers—new models of care and technology must be explored to meet the needs of all patients with allergies.
To meet healthcare demands and address these inequities, our Food Allergy Nurses Interest Group (FANI) has proposed creating a Certified Allergy Nurse Educator role (Kelly et al., 2022). FANI provides a scholarly forum for registered nurses to enhance professional collaboration, advancement, and knowledge sharing in the subspecialty of food allergy to improve health outcomes and quality of life for those living with food allergies. FANI nurses published an article in Allergic Living Magazine online, aimed at laypeople, which is widely read by individuals managing food allergies and their caregivers. Allergic Living offers in-depth coverage of issues facing families and individuals dealing with severe food allergies and asthma. We outlined potential benefits of establishing an ANE role that would meet the needs of providers, patients, and caregivers. The article was accompanied by a brief survey to gather readers’ feedback since its publication in April 2022. We found the collected data very valuable because it helps inform future steps for developing the allergy specialty and the ANE role within the nursing profession, as we aim to optimize resources and improve care delivery and outcomes—in this case, the prevention and management of allergies in the growing number of affected individuals living in America.
Methods
We used an online stakeholder market analysis survey to better understand the public’s perception of the proposed ANE role. An informal survey was created by nurses involved in writing the article for publication in Allergic Living in April 2022. It included three main questions: state/country, interest in the ANE role, and respondents’ roles or relationships to allergies, with instructions to select all applicable categories. Participants could also leave comments and provide contact information to receive updates about the ANE role. An optional survey was available at the end of the article for readers to voluntarily offer feedback on the role. Although this was not an IRB-approved research study, all data remained confidential, de-identified, and were reported in aggregate. Data were analyzed in an Excel database and presented as descriptive statistics with frequencies reflecting participants’ responses.
Results
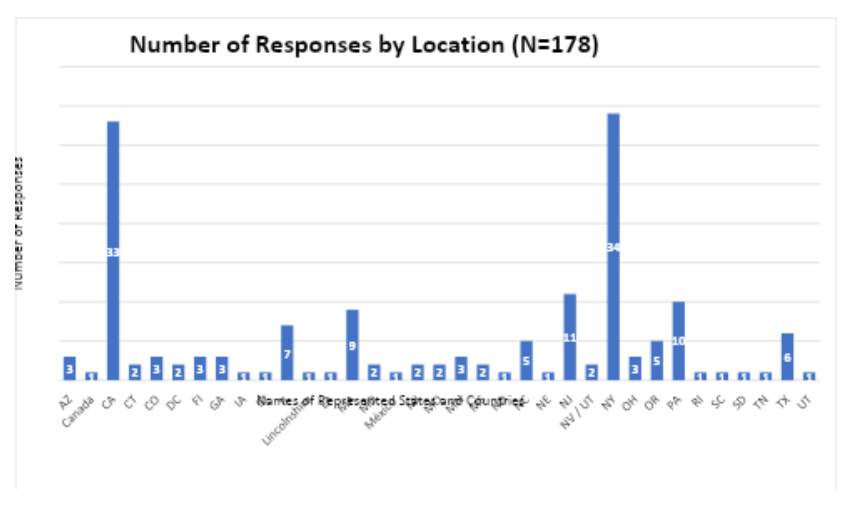
The survey received 179 responses, with one removed due to duplication. A total of 178 responses were included in the analysis. Most respondents were from New York and California, but responses from 36 states were represented. Additionally, a few responses came from Canada, Mexico, and Lincolnshire in England. The breakdown by location is included in Figure 1.
Figure 1. Responses by Geographic Location [AUTHORS: The bottom axis of this graph has overlapping text - can you please fix this and send an updated image that I can insert? Thanks!]
Participants' responses to the question about their role or their relationship to allergies showed that many identified with more than one category. However, most identified as RNs (101, 57%) and as patients with food allergies or their caregivers (98, 55%). Other combined categories (28, 15%) included healthcare professionals, Medical Doctors or Doctors of Osteopathy, Board Certified Allergy & Immunology physicians, Licensed Vocational Nurses (LVNs) or Licensed Practical Nurses (LPNs), and other specialties (Figure 2).
Figure 2. Participant’s role in and/or relationship to allergies
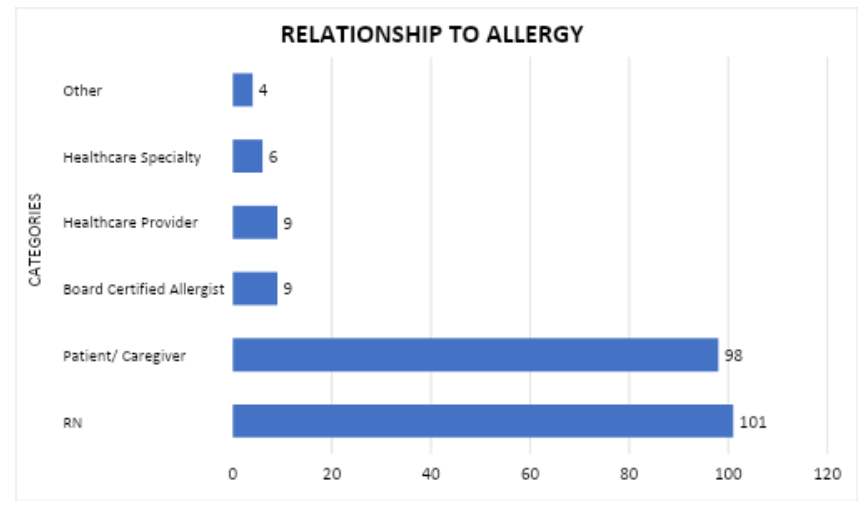
*Note: Respondents could select more than one category. RN (Registered Nurse); Patient / Caregiver (patient with food allergies and/or their caregiver); Healthcare Provider (MD/DO non-allergist, Nurse Practitioner, Physician Assistant); Healthcare Specialty (Registered Dietitian, Nutritionist, Licensed Social Worker, etc.); Other (LPN, LVN, and non-healthcare related).
Respondents could select more than one answer when asked about their interest in the ANE role. 98 (55%) nurses expressed interest in becoming certified allergy nurse educators; 83 (47%) patients/caregivers and 34 (19%) healthcare professionals supported the ANE role; with 19 (11%) interested in piloting the role, and 15 (8%) in hiring an ANE.
Figure 3. Level of Interest in ANE Role
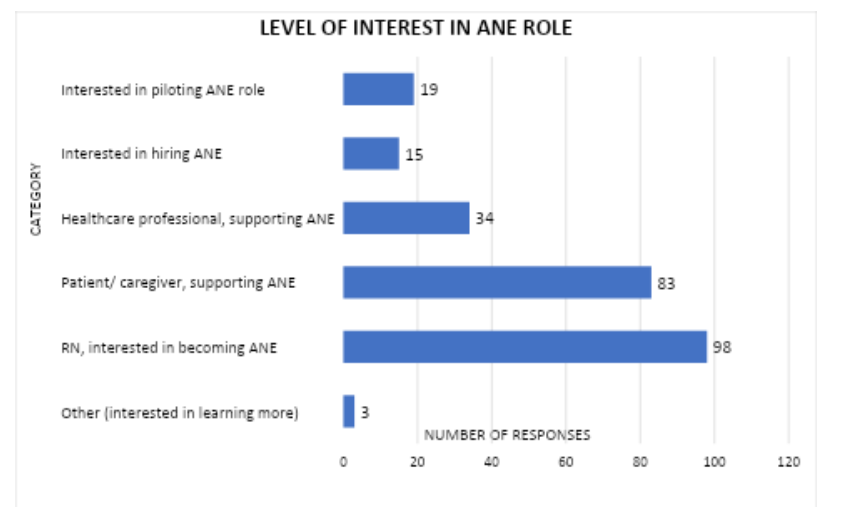
Note: N=178. Respondents had an option to “check all that apply” categories.
Finally, 90 (51%) of respondents left comments showing strong support for the idea of certified allergy nurse educators (ANEs). The main themes that emerged included: 1) certification and training; 2) importance of ANE; 3) patient advocacy and education; 4) personal experiences; 5) desire for implementation; and 6) interest and support.
Several commenters express a desire for certification and training programs specifically tailored to allergy nursing. They have shown interest in becoming certified ANEs to improve their ability to care for patients with allergies, as evidenced by their comments offering assistance to develop a certification and inquiring about available courses related to this role. They also express interest in becoming certified ANE. Allergists support the ANE role, believing it would bring some level of standardization to care. Some mention that nurses already spend extra time taking on this important role, and streamlining this process along with adding some standardization would optimize it for these nurses while providing other interested nurses with a clear pathway into the ANE role.
The commenters emphasized the vital role that ANEs would play in supporting patients with allergies, including those in under-resourced areas. They highlighted the challenges faced by families managing food allergies and the need for expert guidance, believing that ANEs could help with allergy prevention and self-care skills, especially for conditions that often coexist with asthma and allergies. Additionally, they could offer assistance for less understood conditions like eosinophilic esophagitis (EOE) and food protein-induced enterocolitis (FPIES). Some comments focused on providing allergy education to under-resourced communities to prevent medical emergencies and hospitalizations, as well as helping families experienced in food allergies navigate new questions related to groundbreaking research, novel treatments, medications, and additional diagnoses that may emerge. It was also noted that food allergies impact all aspects of a patient’s life, including home, school, dining out, sports, church, and more.
The role of ANEs goes beyond medical care. They would also advocate for patients, educate families, and offer practical advice. Families managing food allergies often have questions, encounter new research, and face additional diagnoses. ANEs could help guide them through these challenges. Mental health support and proper medication administration are also key parts of allergy management. Several comments emphasized the patient advocacy and education roles of the proposed ANE position. One commenter mentioned they would have appreciated someone like ANE who could see the big picture, understand anxiety, explain medical information clearly, direct them to better resources, and provide practical advice on how to move forward, what questions to ask, and what to consider over time—rather than trying to piece everything together and research extensively on their own, which can lead to mistakes, such as avoiding foods unnecessarily. Others viewed ANE as someone who can help families adapt to living with food allergies more quickly than trying to figure it out alone, preventing feelings of isolation. They also believed ANE would assist primary healthcare providers with more hands-on treatments or prevention strategies for their patients.
Several commenters shared their personal journeys as parents of children with severe food allergies. Some used their RN experience to navigate life successfully. They expressed disappointment that there is no certification option for communicating expertise, especially given the positive impact ANEs could have. One parent shared that her child was born with multiple, severe food allergies, and she used her RN experience and education to adapt to every aspect of their life. Her daughter never experienced anaphylaxis because she learned and applied all the best practices and became a content expert, while other parents without healthcare backgrounds had to “fumble” their way through finding answers online after their child was discharged from the hospital due to a first-time reaction.
Commenters expressed enthusiasm for the idea of ANEs and stressed the importance of establishing their standardized role. Some shared the challenges they faced when seeking information and guidance after their child’s diagnosis. Several comments indicated that ANEs could offer a framework and holistic support. For instance, one person mentioned they would have greatly appreciated help from someone in an ANE role when their son was first diagnosed. Other parents shared that they felt shocked, terrified, and completely unprepared for their new responsibilities as parents of a “little one” diagnosed with multiple food allergies at eight months old. They were surprised that the ANE role had not yet been implemented, especially considering current statistics showing 1 in 13 children have food allergies. One nurse, who is a parent of a son with FPIES and allergies—including managing her own allergies—said she could not do it without being an RN and expressed a strong need for ANEs.
Many expressed interest in getting involved or pursuing a career as an ANE when available. The idea resonated deeply with nurses, physicians, parents, and individuals directly affected by food allergies. One nurse, who is also a parent of a child with over 30 food allergies, said that ANE would be her dream job and is of utmost importance. Allergists showed interest in having a specialized team of professionals to best support their patients and families, stating that ANE would be a valuable addition to that team. Additionally, they mentioned that the community outreach an ANE could provide would be especially helpful to groups like schools and early learning centers.
In summary, the comments demonstrated strong support for certified allergy nurse educators (ANEs), highlighting the need for certification, patient advocacy, and practical guidance. Personal experiences emphasize the importance of this role in helping families with food allergies, including those in underserved and rural communities.
Discussion
Since most of Allergic Living's readership consists of patients with allergies and/or their caregivers, it was expected that the majority of respondents would come from these groups, followed by nurses, many of whom also identified with the latter. This could also explain the high number of nurses responding to the survey. Allergic Living circulated their publication containing the article on various social media platforms, which was shared and reshared by different groups and individuals. As a result, it may have reached an audience beyond the intended layperson, leading to several responses from professionals working in medicine and allied health.
The richness of qualitative data contained in the comments complemented the quantitative data gathered about respondents’ common desire to see the ANE role become the new standard of care for people living with allergies. It is also promising that respondents from all 36 states and three international locations selected at least one way to support this proposed role, such as piloting the ANE role, hiring an ANE in their practice, or pursuing the certification (once available).
An Allergy Nurse Educator role, including registered nurses (RN) and advanced practice registered nurses (APRN) with specialized allergy training, would help meet patients' needs for affordable and timely allergy care across the United States, utilizing existing telehealth tools as necessary. Based on feedback from the survey, the Allergic Living article, and the existing allergy nursing competency document from the British Society for Allergy & Clinical Immunology (BSACI, 2024), the ANE could offer in-person and/or remote education, support, and advocacy for patients with allergies and their caregivers. Some key responsibilities may include:
- Patient Education: inform patients and their families about allergy management, preventing allergic reactions, and responding to anaphylaxis emergencies.
- Care Coordination: Collaborate with allergists and other healthcare providers to create comprehensive care plans for patients with allergies.
- Community Outreach: Host workshops, seminars, and community events to increase awareness about allergies and anaphylaxis.
- Resource Development: Develop educational materials, such as handouts, videos, and online resources, to support patients and caregivers.
- Professional Development: Keep current with the latest research and advancements in allergy care, and share this knowledge with colleagues and patients.
- Support Groups: Lead support groups for patients and families managing allergies to offer emotional and practical assistance.
Incidental finding
Additionally, ANE professionals need to have several skills and qualifications to perform effectively in their roles. These may include, but are not limited to:
- Clinical Expertise: Extensive knowledge of allergy and immunology, including diagnosis, treatment, and management of allergic conditions.
- Educational Skills: Excellent communication and teaching abilities to clearly explain complex medical information to patients and caregivers.
- Empathy and Compassion: Ability to offer emotional support and understanding to patients and families dealing with the challenges of living with allergies.
- Advocacy: Skills in supporting patients' needs and rights within the healthcare system and community.
- Cultural Competence: Ability to engage with diverse groups and deliver culturally mindful care and education.
An Allergy Nurse Educator can play a vital role in enhancing patient outcomes by delivering thorough education, support, and advocacy. By empowering patients and caregivers with knowledge and resources, ANEs can help decrease the risk of allergic reactions and improve the quality of life for those living with allergies.
Recommendations
The National Nursing Workforce Survey, a nationwide survey of the entire U.S. nursing workforce conducted by the National Council of State Boards of Nursing (NCSBN) and the National Forum of State Nursing Workforce Centers (Forum), does not include nurses working in allergy, asthma, and immunology areas (Smiley et al., 2023). Currently, it is unknown how many nurses practice in allergy because no formal studies have examined the landscape of allergy nursing. Therefore, a more formal assessment of the current allergy nursing workforce is highly desirable. It is also recommended that NCSBN and the ANA Enterprise include allergy, asthma, and immunology as a category in their future surveys. Nurses working in allergy already serve as informal allergy nurse educators, often gaining experience on the job or learning from their peers through allergist-driven organizations like the American Academy of Allergy, Asthma, and Immunology (AAAAI) and the American College of Allergy, Asthma & Immunology (ACAAI), where some of these nurses hold memberships within their Allied Health category. The American Society of Allergy Nurses (ASAN) also offers continuing education opportunities at their annual conferences, primarily reaching nurses on the West Coast. Food Allergy Research and Education (FARE), a nonprofit patient advocacy organization, offers an online course for Registered Dietitians (RDs), which some nurses find helpful; however, it does not fully address the needs of nurses interested in allergy nursing, nor does it offer the American Nurses Credentialing Center (ANCC)-approved continuing professional development credits or allergy nursing certification. For the Advanced Nurse Educator (ANE) role to develop and for allergy nursing to become a recognized specialty, a more coordinated effort is needed to bring together nurses already working in allergy and those interested in joining within a single, nurse-led organization. This would enable collective advocacy and promotion of the ANE role, define the minimally required competencies and standards of care, and support nurse-led allergy research, patient advocacy, professional networking, education, and collaboration with external professional groups.
Conclusion
In the effort to meet healthcare needs and reduce health disparities among people with allergies, the Food Allergy Nurses Interest Group (FANI) has proposed creating a Certified Allergy Nurse Educator (ANE) role, similar to a diabetes nurse educator. Currently, there is no formal certification or requirement for nurses specializing in allergy in the United States. Our publication, Allergic Living (2022), and the data presented in this article underscore the need for this innovative nursing role, aiming to optimize resources, improve care delivery, and enhance outcomes for patients and caregivers. We are committed to making this vision a reality for all nurses who are passionate about caring for patients with allergies and related conditions.
Authors
Olga Kagan, PhD, RN, FHIMSS, FAAAAI
Email: okagan@molloy.edu
ORCID ID:
Olga Kagan is a dedicated nurse scientist, educator, and entrepreneur with a mission to advance food allergy management, education, and policy. Specializing in innovation and informatics, she brings transformative approaches to healthcare, drawing from experiences in infectious disease, critical care, and 9/11 related occupational and environmental health. Dr. Kagan actively imparts her knowledge to graduate students at two New York-based universities, serves on boards and as a peer reviewer, mentor, and invited speaker in professional organizations like HIMSS, ANA, SONSIEL and ENRS. As a leader of the Food Allergy Nursing Interest Professional Group (FANI), providing a scholarly forum for nurses in food allergy and anaphylaxis, she continues to shape the landscape of allergy-informed nursing. She has been volunteering with several AAAAI committees. Dr. Kagan is a recipient of multiple awards for her impactful contributions to research, leadership, and mentorship.
Susan Kelly, BSN, RN
Email: sheimkelly@gmail.com
ORCID ID:
Susan Kelly received her Bachelor of Science in Nursing from the University of Scranton in 1996. She is pursuing her graduate degree in Public Health at Hofstra University. Susan is the Nurse Manager at Happy and Healthy Pediatrics in Mineola, NY. Her clinical background as a nurse in the hospital setting includes working in the areas of general medicine, cardiology, electrophysiology, intensive care, and the emergency room. She also worked as a nurse in the primary care setting for a board-certified allergist and immunologist.
References
American Board of Allergy and Immunology. (n.d.) About ABAI. https://www.abai.org/aboutabai.asp
British Society for Allergy & Clinical Immunology. (2024). Allergy nurse competency document. https://www.bsaci.org/wp-content/uploads/2020/02/AllergyNurseCompetences_Edition1_Nov2014-3.pdf
Centers for Disease Control. (2023, January 26). More than a quarter of U.S. adults and children have at least one allergy. https://www.cdc.gov/nchs/pressroom/releases/20230126.html
Gallup. (January 22, 2024). Ethics ratings of nearly all professions down in U.S. https://news.gallup.com/poll/608903/ethics-ratings-nearly-professions-down.aspx
Ho, F., Zheng, C., Frazier, M., Nimmagadda, S., Gupta, R., & Bilaver, L. (2024). Geographic variability of medicaid acceptance across allergists in the United States. Journal of Allergy & Clinical Immunology, 153(2). https://doi.org/10.37765/ajmc.2024.89588
Kelly, S., Kagan, O., Howard-Ruben, J., Doucette, J., Weiss, K., Koo, L., Bolten, A., & D’Amato, C. (2022). Food allergy nurses interest group. Why we need certified allergy nurse educators. Allergic Living. https://www.allergicliving.com/2022/04/04/why-we-need-certified-allergy-nurse-educators/
Ng, A. E., & Boersma, P. (2023, January 26). Diagnosed allergic conditions in adults: United States, 2021. NCHS Data Briefs, 460. https://doi.org/10.15620/cdc:122809
Smiley, R. A., Allgeyer, R. L., Shobo, Y., Lyons, K. C., Letourneau, R., Zhong, E., Kaminski-Ozturk, N., & Alexander, M. (2023). The 2022 National Nursing Workforce Survey. Journal of Nursing Regulation, 14(1). https://doi.org/10.1016/S2155-8256(23)00047-9
Zablotsky, B., Black, L. I., & Akinbami, L. J. (2023, January 26). Diagnosed allergic conditions in children aged 0–17 years: United States, 2021. NCHS Data Briefs, 459. https://doi.org/10.15620/cdc:123250

