Applications using artificial intelligence (AI) have shown potential to assist nurses with patient care activities. Nurses are in a position to influence the judicious use of AI that best supports practice needs in the future by participating in the design, development, testing, and evaluation of solutions. Thus, it is important for nurses at all levels to have a general understanding of the key concepts, potential benefits of AI, and unintended consequences as they consider its adoption in clinical practice. This article includes introductory level discussion about data management and components of AI that include real-world cases in use by nurses and offers implications for nursing practice.
Key Words: Data analytics, predictive analytics, artificial intelligence, augmented intelligence, nursing informatics, clinical informatics, machine learning, data management, data literacy, robotics, patient generated health data
Some may believe that we have too much data to even be useful at the point of care.With the increasing amount of data available in the healthcare setting, coupled with new and emerging technologies implemented on a daily basis, nurses are presented with many opportunities to apply data, information, and knowledge to practice in novel ways. Data collection from the electronic health record (EHR) has grown exponentially in the past decade. Improved methods of data sharing facilitate data transparency. New capabilities for data analytics allow processing of large data sets needed to answer complex clinical questions and potentially improve patient care. Some may believe that we have too much data to even be useful at the point of care. Thus, nurses have an abundance of data at their fingertips, and new technologies must be applied to render them usable.
AI (Davenport & Kalakota, 2019) has shown potential to assist clinicians in patient care...Computers and other automated systems can manage and process the large amounts of data now available. One broad concept related to health data that has gained attention in recent years is artificial intelligence (AI), which is the idea that machines can execute tasks similar to humans. AI (Davenport & Kalakota, 2019) has shown potential to assist clinicians in patient care (also called augmented intelligence), especially in some administrative functions. But while some studies suggest that AI can perform just as well, or even better, than clinicians in diagnostic tasks, it will still be many years before we see routine use of AI in clinical practice (Panch, Mattie, & Celi, 2019).
...it is important for nurses at all levels to have a general understanding of AI and consider its use in clinical practice.Specific to the nursing profession, AI can be used as part of daily workflows and has the potential to eliminate inefficiencies that contribute to existing clinical burnout. As we move closer to realizing the benefits of AI in healthcare, it is important for nurses at all levels to have a general understanding of AI and consider its use in clinical practice. In particular, nurses can influence the thoughtful use of AI that best supports practice needs in the future. In this article, we begin with a review of key concepts, breakdown the components of AI using real-world nursing use cases, make the case for increased use of the term augmented intelligence, and provide strategies for ongoing nursing engagement with AI technologies.
Key Concepts
To offer a foundation for data literacy, we begin with a review of the components of the Data, Information, Knowledge and Wisdom (DIKW) Model (Nelson, 2020). This includes a description of the types of analytics processes in healthcare, based on Nelson’s (2020) model, and introduction of the three branches of AI. This foundational knowledge can be useful to support nursing involvement in AI related activities.
DIKW Model
Data
Data, also called data elements, are a collection of facts that are generally unorganized.Data, also called data elements, are a collection of facts that are generally unorganized. In healthcare, the biggest source of data, typically in the form of text or pixel, is the EHR. There are many other ways to obtain data electronically. They may be generated and collected by other providers, payers, and pharmacies using clinical technologies and tools that may not be connected to the EHR. Recently, there has been a concerted effort to find scalable ways to obtain data from patients in an electronic fashion using monitoring devices, sensors, or mobile health applications (Adler-Milstein & Nong, 2019). One example of a data element is a blood pressure reading. Ultimately, the collection of data in healthcare must extend beyond the hospital encounter and consider the entire landscape of available data that may contribute to a patient’s good health.
Information
Health data are tied to a human being at a particular point in time and there may be multiple types of data in a patient’s timeline.Information is how we understand facts or data within context in a structured way. In healthcare, the context is specifically information to support clinical care needs. Health data are tied to a human being at a particular point in time and there may be multiple types of data in a patient’s timeline. Given the amount of health data available, the challenge is to find meaningful information and surface that information at the point in the clinical workflow where it will be most useful. This requires not only contextualizing, but summarizing and analyzing data, to uncover relationships that produce logical meaning for the clinician. A group of blood pressure readings that are organized in a temporal fashion alongside other symptom data elements in a way that supports interpreting the significance of the readings is an example of information.
Knowledge
Knowledge might be represented as a set of rules to facilitate understanding...Knowledge is a way to formalize the relationships between the data and information. It is the result of understanding the implications of the information. Knowledge might be represented as a set of rules to facilitate understanding, such as indicating when a blood pressure may be out of range for a particular diagnosis.
Wisdom
Wisdom is the application of data, information, and knowledge to make decisions, implement nursing actions, and improve healthcare processes. Wisdom is also connected to the ability to integrate data with professional values and apply data to human problems (Whalen et al., 2016). An example is the provision of culturally appropriate, low-salt diet education materials to a patient with uncontrolled blood pressure.
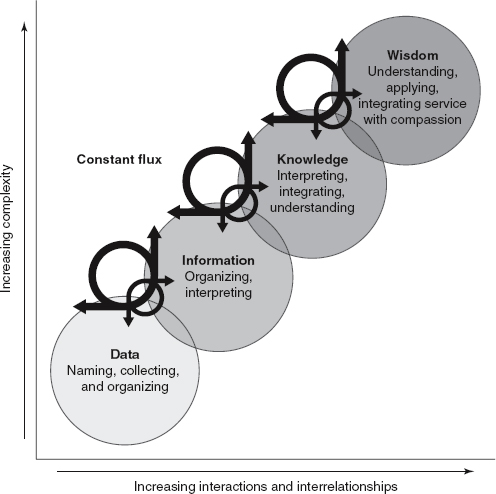
Depicted in the Figure, the interrelationship between data, information, knowledge, and wisdom is represented by the theoretical framework: Data, Information, Knowledge and Wisdom Model (DIKW Model) by Ramona Nelson (2020). This framework serves as the foundation for explaining the role of AI systems in generating knowledge (Cato, McGrow, & Rossetti, 2020).
Figure. Revised Data Information Knowledge Wisdom Model – 2013 Version
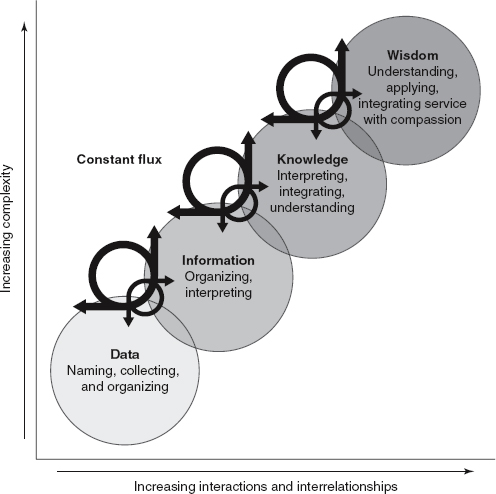
(Figure reprinted with permission from Ramona Nelson, Copyright © 2013, Ramona Nelson Consulting at ramonanelson@verizon.net. All rights reserved.)
Analytics
There are four main levels of data analytics that differ in the level of complexity of analysis.There are four main levels of data analytics that differ in the level of complexity of analysis. Descriptive, diagnostics, and predictive analytics are commonly used in healthcare, but prescriptive applications are in their infancy. Below are brief descriptions of these concepts.
- Descriptive Analytics is the most basic form of analytics. It is a way to explain what happened using data. It is beneficial for exploring the data. This type of analysis is more comprehensive and focuses on what the data are describing in real time.
- Diagnostic Analytics takes analysis a step further to understand why something happened within the data collected. This is accomplished by using the data to identify the root cause and then isolating any confounding information. With a health data set, symptom data and patient history data can be used to generate diagnosis for patients.
- Predictive Analytics is used in forecasting what is likely to happen. By looking at historical patterns in the data, particular outcomes may be predicted. Predicted outcomes may be presented to clinicians to assist with decision-making. Once identified, decisions may be automated using algorithms and technology.
- Prescriptive Analytics is the most advanced level of analytics. This method uses the data to recommend actions and strategies based on the forecast. Various outcomes are tested to identify the best result, given the data provided.
Artificial Intelligence
AI is a branch of computer science with many sub-fields...Artificial Intelligence is, very simply, an umbrella term for a set of tools that make computers ‘smarter.’ AI is a branch of computer science with many sub-fields, all of which strive to mimic some aspect of human intelligence. In the healthcare domain, AI-based applications are used to surface information from the EHR to clinicians and provide correlations from the data that might not be easily discoverable given current data views (Braun, Hummel, Beck, & Dabrock, 2020). Below we briefly describe three types of AI.
- Machine Learning is currently the most common subset of AI used in healthcare. This statistical method enables a system to learn from data without explicitly being programmed. It can be used to automate predictive analytics and can support precision medicine activities that tailor treatments to a specific patient care profile. For instance, tools such as the Communicating Narrative Concerns Entered by RNs (CONCERN) clinical decision support system can predict patient risk for clinical deterioration (Cato, McGrow, & Rossetti, 2020). Some EHR software vendors have prebuilt machine learning models as part of their products, such as the Cerner EHR that uses AI for A1C risk predictions (McGrail, 2020).
- Natural Language Processing (NLP) is an AI specialization area used to process and analyze large amounts of human language data in a textual format. NLP enables a computer to read and understand data by mimicking natural language. In healthcare, it is used to understand and classify clinical documentation. NLP systems can analyze unstructured clinical notes on patients, give insight into understanding quality, and ultimately, provide better results for patients (Sheikhalishahi et al., 2019).
- Computer Vision is a method of using advanced AI algorithms to assist with image processing that reads in real time. It is used to discover patterns in images and videos for tasks that require a trained eye, thereby increasing accuracy and saving time for clinicians. This method can be used to detect and interpret early symptoms through physiologic monitoring or detection of patient movement (Glancova et al., 2021).
Augmented Intelligence is a practical way to conceptualize the AI assistive role in human-decision making. The term augmented intelligence is used synonymously with AI (Skiba, 2017). This term emphasizes the fact that AI technology is used to enhance or amplify human intelligence instead of replacing it. In the context of nursing practice, augmented intelligence highlights efficiencies that can be gained from effective use of data to enable all nurses to practice at the top scope of licensure.
Potential Benefits of AI
AI-based technologies have the potential to assist nurses in many tasks, freeing time to focus on patient care.AI-based technologies have the potential to assist nurses in many tasks, freeing time to focus on patient care. Tasks accomplished by an AI-enabled robot or AI-based software support include lifting, staffing assignments, real-time documentation, and the review of patent generated health data (e.g., health monitoring app on a smartphone). Below are some examples of these technologies.
- Robots. Nurses injure themselves at high rates while assisting, turning, and lifting patients (Kanaskie & Snyder, 2018). AI-enabled robots can assist nurses when they need to move a patient such as with the robot for interactive body assistance (RIBA) robot from Japan which can lift patients up to 80 kilograms. (Goeldner, Herstatt, & Tietze, 2015).
- Staffing. The assignment of patient care load has long stumped nurse managers. The savvy nurse understands how to distribute patients equally at the beginning of a shift, but it is impossible to know who will be transferred or how many patients will be admitted during a particular shift. Software can analyze patterns of patient transfer and possible admissions to predict the characteristics of unit census over time. This level of analysis supports unit functions and provides transparency for unit staffing.
- Documentation Improvement. It is highly anticipated that AI solutions will soon be used to reduce the amount of time spent by nurses charting in front of a computer. This includes limiting the search for relevant data for clinical decision-making. Similarly, ambient voice enabled AI using smart speakers can be used to convert spoken words to clinical notes and documentation.
- Patient Generated Health Data. There is a tidal wave of health-related data that patients collect using smart watches, apps, and other devices. Patients are already trying to share these data with providers, but a new, voluminous data source can be challenging for busy clinicians to review. AI software can efficiently filter these new data sources given the care context, present it to the nurse in a meaningful way, and allow the visualization of important trends when integrated into the EHR.
Unintended Consequences
For AI to be impactful and work as promised, it is crucial that nurses participate in AI design, development, and implementation. AI solutions promise to provide a number of improvements for healthcare, patients, and specifically nurses in practice. However, some have raised concerns about the use of AI in healthcare and potential impact to nurses and patient care. Several unintended consequences raised by clinicians are: 1) Job security, or positions replaced by technology (Ronquillo et al., 2021), 2) Trust needed to understand the mechanisms that lead to recommendations, and 3) Diversity, equity, and inclusion concerns about the applicability of AI solutions to a diverse set of patients and clinicians (Asan, Bayrak, & Choudhury, 2020). To increase nursing engagement, it is important to address concerns related to AI use and socialize mitigation strategies (Gianfrancesco, Tamang, Yazdany, & Schmajuk, 2018). For AI to be impactful and work as promised, it is crucial that nurses participate in AI design, development, and implementation. We briefly consider these concerns below.
Job Security
...one of the first concerns raised is the idea that software and robots may eliminate nursing jobs. When many nurses hear about the benefits of AI, one of the first concerns raised is the idea that software and robots may eliminate nursing jobs. Given the novelty of AI technologies and their application in healthcare, a computer replacing the human being on a large scale is a long way off. Although there have been tremendous advancements and computers can now do some very specific tasks much better than a human, patient care aspects such as empathy and human touch cannot be replaced by AI. For job roles, AI as a way to improve nursing care should be considered as augmentation instead of replacement. For example, for a nurse in the inpatient setting, a robot has the potential to find all of the supplies needed before a patient arrives to the room. The availability of this service could be a tremendous time-saver for nurses. AI will work best when it is helping nurses do their job, thus freeing more time to spend with patients and their caregivers.
Trust
...AI should make clinical sense and be used to solve a problem in need of solving.Nurses at the bedside are ultimately responsible to assure that a treatment is safe and appropriate (e.g., the five rights). Since AI can be used to recommend care, nurses must be able to trust that the AI recommendations are sound. For example, if an AI system identifies individuals at high risk for falling at home, the nurse should have information about the performance of the AI algorithm and know which data from the EHR are used to identify patients at risk. In addition to understanding the AI underpinnings, the AI should make clinical sense and be used to solve a problem in need of solving. Including nurses in AI building and testing can provide ideal uses cases, and thus increase nursing knowledge and buy-in of this technology.
Diversity, Equity, and Inclusion.
There have been issues with some AI based software that perpetuate biasNurses are in a position to address inequities and ensure that a diverse set of patients receive quality and safe care. There have been issues with some AI based software that perpetuate bias (Röösli, Rice, & Hernandez-Boussard, 2021). For example, there are types of facial recognition software that are not able to tell different African American faces apart from others. Nurses should inquire as to whether AI has been used on diverse populations, including but not limited to populations of varied age, sex, and race. By including nurses in the design of AI solutions, there is the ability to reduce algorithm bias and avoid potential inequities.
Implications for Nursing Practice
By participating in AI activities, nurses can complement their strong critical thinking and problem-solving abilities...The emergence of big data and the application of AI for data management offer many opportunities for nurses. Technological advances and improved access to data can create more efficient processes and afford greater insight into patient care, thereby augmenting intelligence. By participating in AI activities, nurses can complement their strong critical thinking and problem-solving abilities with exposure to advanced technical knowledge and data management skills.
In the healthcare domain, most work occurs prior to the AI modeling.In addition to understanding the general concepts related to data analytics and AI, there are opportunities for nurses to get involved in the process at every stage. In the healthcare domain, most work occurs prior to the AI modeling. The first step, understanding the clinical problem to be solved, is the most important area for contribution by nurses, given that they are keenly aware of the most pressing issues in patient care. Participation by nurses can inform which clinical questions need to be answered and which complex decisions lend themselves to solutions using AI. This requires nurse input in meetings where AI decisions are made or time for nurses to brainstorm and collaborate with technology developers. As a next step, nurses can also contribute to interdisciplinary teams that design and develop projects for quality improvement purposes or other safety initiatives.
...nurses are also integral in the testing and evaluation of AI solutions.Once developed, nurses are also integral in the testing and evaluation of AI solutions. At this stage, nurses can assess for bias in algorithms and determine the potential impact on patient care. Nurses can also influence the timing of the AI solution by examining its placement within clinical workflows and determine adjustments appropriate to nursing practice. AI should be measured in terms of patient outcomes, and nurses are well positioned to evaluate positive care improvements, suggest implementation in other care settings, and disseminate evidence within the healthcare domain as a whole. The check list of activities in Table 1 below may be helpful nurses who have interest in AI activity involvement.
Table 1. Checklist for Nurse Participation in Artificial Intelligence
| These activities can be useful on a general level and in a specific employment setting:
|
In addition, the resources listed in Table 2 can be useful to help nurses stay abreast of new activities and evidence about the use of AI in nursing practice:
Table 2. Helpful Resources
| Resource | URL |
| Nursing Knowledge: Big Data Science Conference | Available: https://www.nursing.umn.edu/2021-nursing-knowledge-big-data-science-conference |
| Artificial intelligence in nursing: Priorities and opportunities from an international invitational think-tank of the Nursing and Artificial Intelligence Leadership Collaborative (Ronquillo et al., 2021) | Available: https://onlinelibrary.wiley.com/doi/10.1111/jan.14855 |
| World Health Organization: Big data and artificial intelligence |
Conclusion
...AI should be seen as a method to augment nursing care. Artificial intelligence has the potential to benefit the nursing workforce by creating more efficient processes, delivering better care for patients, saving lives, and ultimately changing the way that nurses practice. Thus, AI should be seen as a method to augment nursing care. Nurses are in a position to influence the design and implementation of AI solutions. We believe that nurses at all levels should have a basic understanding and be able to comfortably converse about AI solutions and actively engage in efforts for their judicious use in practice. Use of AI technologies in nursing practice can facilitate a greater good for our profession and for the populations we serve.
Authors
Victoria L. Tiase, PhD, RN-BC, FAMIA, FAAN
Email: vtiase@nyp.org
Victoria L. Tiase is the Director of Research Science at New York-Presbyterian Hospital and an Assistant Professor of Health Informatics at Weill Cornell Medicine. She supports a range of clinical information technology projects related to patient engagement and the integration of patient generated health data into clinical workflows. She is the chair of the HIMSS Nursing Informatics Committee and serves on the boards of AMIA, NODE.Health, and the CARIN Alliance. Recently, she was appointed to the National Academy of Medicine Committee on the Future of Nursing 2020-2030. She completed a BSN at the University of Virginia; MSN at Columbia University; and PhD at the University of Utah.
Kenrick D. Cato, PhD, RN, CPHIMS, FAAN
Email: kdc2110@cumc.columbia.edu
Kenrick Cato is a Nurse Researcher/Assistant Professor/ Assistant Professor of Clinical Informatics for New York-Presbyterian Hospital and Columbia University School of Nursing and the Department of Emergency Medicine for the Columbia University Irving Medical Center, respectively. Dr. Cato's program of research focuses on the mining of electronic patient data to support clinical decision making. He obtained a Bachelor of Nursing and a PhD in Clinical Informatics from Columbia University. Recently, Dr. Cato served as the co-chair for the American Medical Informatics Association’s Clinical Informatics Conference, which attracts participants from the United States and beyond.
References
Adler-Milstein, J., & Nong, P. (2019). Early experiences with patient generated health data: health system and patient perspectives. Journal of the American Medical Informatics Association, 26(10), 952-959. https://doi.org/10.1093/jamia/ocz045
Asan, O., Bayrak, A. E., & Choudhury, A. (2020). Artificial intelligence and human trust in healthcare: Focus on clinicians. Journal of Medical Internet Research, 22(6), e15154. https://doi.org/10.2196/15154
Braun, M., Hummel, P., Beck, S., & Dabrock, P. (2020). Primer on an ethics of AI-based decision support systems in the clinic. Journal of Medical Ethics, 0, 1-8. https://doi.org/10.1136/medethics-2019-105860
Cato, K. D., McGrow, K., & Rossetti, S. C. (2020). Transforming clinical data into wisdom: Artificial intelligence implications for nurse leaders. Nursing Management, 51(11), 24-30. https://doi.org/10.1097/01.NUMA.0000719396.83518.d6
Davenport, T., & Kalakota, R. (2019). The potential for artificial intelligence in healthcare. Future Healthcare Journal, 6(2), 94–98. https://doi.org/10.7861%2Ffuturehosp.6-2-94
Gianfrancesco, M. A., Tamang, S., Yazdany, J., & Schmajuk, G. (2018). Potential biases in machine learning algorithms using electronic health record data. JAMA Internal Medicine, 178(11), 1544. https://doi.org/10.1001/jamainternmed.2018.3763
Glancova, A., Do, Q.T., Sanghavi, D.K., Franco, P.M., Gopal, N., Lehman, L.M., Dong, Y., Pickering, B.W., Herasevich, V. (2021). Are we ready for video recognition and computer vision in the intensive care unit? A survey. Applied Clinical Informatics, 12(1), 120-132. https://doi.org/10.1055/s-0040-1722614
Goeldner, M., Herstatt, C., & Tietze, F. (2015). The emergence of care robotics—A patent and publication analysis. Technological Forecasting and Social Change, 92, 115-131. https://doi.org/10.1016/j.techfore.2014.09.005
Kanaskie, M. L., & Snyder, C. (2018). Nurses and nursing assistants decision-making regarding use of safe patient handling and mobility technology: A qualitative study. Applied Nursing Research, 39, 141-147. https://doi.org/10.1016/j.apnr.2017.11.006
McGrail, S. (2020, May 21). How EHRs are leveraging artificial intelligence capabilities. Networking News. Retrieved from: https://hitinfrastructure.com/news/how-ehrs-are-leveraging-artificial-intelligence-capabilities
Nelson, R. (2020). Informatics: Evolution of the Nelson Data, Information, Knowledge and Wisdom Model: Part 2. OJIN: The Online Journal of Issues in Nursing, 25(3). https://doi.org/10.3912/OJIN.Vol25No03InfoCol01
Panch, T., Mattie, H., & Celi, L. A. (2019). The “inconvenient truth” about AI in healthcare. NPJ Digital Medicine, 2(1), 77. https://doi.org/10.1038/s41746-019-0155-4
Röösli, E., Rice, B., & Hernandez-Boussard, T. (2021). Bias at warp speed: How AI may contribute to the disparities gap in the time of COVID-19. Journal of the American Medical Informatics Association, 28(1), 190-192. https://doi.org/10.1093/jamia/ocaa210
Ronquillo, C. E., Peltonen, L. M., Pruinelli, L., Chu, C. H., Bakken, S., Beduschi, A., Cato, K., Hardiker, N., Junger, A., Michalowski, M., Nyrup, R., Eng, S. R., Reed, D. N., Salakoski, T., Salantera, S., Walton, N., Weber, P., Wiegand, T., & Topaz, M. (2021). Artificial intelligence in nursing: Priorities and opportunities from an international invitational think'tank of the Nursing and Artificial Intelligence Leadership Collaborative. Journal of Advanced Nursing, 77(9), 3707-3717. https://doi.org/10.1111/jan.14855
Sheikhalishahi, S., Miotto, R., Dudley, J. T., Lavelli, A., Rinaldi, F., Osmani, V. (2019). Natural language processing of clinical notes on chronic diseases: Systematic review. JMIR Medical Informatics, 7(2), e12239. https://doi.org/10.2196/12239
Skiba, D. J. (2017). Augmented intelligence and nursing. Nursing Education Perspectives, 38(2), 108-109. https://doi.org/10.1097/01.nep.0000000000000124
Whalen, K., Bavuso, K., Bouyer-Ferullo, S., Goldsmith, D., Fairbanks, A., Gesner, E., Lagor, C., & Collins, S. (2016). Analysis of nursing clinical decision support requests and strategic plan in a large academic health system. Applied Clinical Informatics, 7(2), 227-237. https://doi.org/10.4338%2FACI-2015-10-RA-0128