Diversity. The changing demographics and economics of our growing multicultural world, and the long-standing disparities in the health status of people from culturally diverse backgrounds has challenged health care providers and organizations to consider cultural diversity as a priority. The purpose of this article is to present a model that will be helpful in providing culturally competent care. The concept of cultural competence is discussed, The Process of Cultural Competence in the Delivery of Healthcare Services Model is described, and a mnemonic to guide in providing culturally competent care is presented.
Key words: culture, diversity, cultural competence, cultural diversity, transcultural health care, cross-cultural health care, transcultural nursing, model of cultural competence, culturally and linguistically appropriate services, racial and ethnic disparities, ethnicity, multicultural health care
Many Faces: Addressing Diversity in Health Care
Diversity. It is a word that means something different to each and every person. The changing demographics and economics of our growing multicultural world and the long-standing disparities in the health status of people from culturally diverse backgrounds have challenged health care providers and organizations to consider cultural diversity as a priority. However, health care providers must realize that addressing cultural diversity goes beyond knowing the values, beliefs, practices and customs of African Americans, Asians, Hispanics/Latinos, Native Americans/Alaskan Natives, and Pacific Islanders. In addition to racial classification and national origin, there are many other faces of cultural diversity. Religious affiliation, language, physical size, gender, sexual orientation, age, disability (both physical and mental), political orientation, socio-economic status, occupational status and geographical location are but a few of the faces of diversity. This article will discuss the concept of cultural competence, describe a model of cultural competence that can be used in the delivery of health care services to address the many faces of diversity, and present a mnemonic to help in asking questions whose responses will facilitate culturally competent care.
Culture and Cultural Competence
The literature is saturated with many definitions of culture. Krober and Kluckhohn (1952/1978) cite over 164 definitions of culture. Late in the 1800s, Tylor (1871) defined culture "as that complex and whole which includes knowledge, belief, art, morals, law, custom, any other capabilities and habits acquired by man as a member of society" (p. 1).
Cultural values give an individual a sense of direction as well as meaning to life.
Cultural values give an individual a sense of direction as well as meaning to life. |
These values are held on an unconscious level. There is a direct relationship between culture and health practices. In fact, of the many factors that are known to determine health beliefs and behaviors, culture is the most influential (Harwood, 1981).
To meet the needs of culturally diverse groups, health care providers must engage in the process of becoming culturally competent. Cross, Bazron, Dennis, & Isaacs (1989) define cultural competence as "a set of congruent behaviors, attitudes, and policies that come together in a system, agency, or amongst professionals and enables that system, agency or those professionals to work effectively in cross-cultural situations" (p. iv). The word competence is used because it implies having the capacity to function effectively.
In 2000, the United States Department of Health and Human Services (DHHS) Office of Minority Health (OMH) released national standards for culturally and linguistically appropriate services (CLAS) as a means to address and correct inequities that exist in the provision of health care to culturally and ethnically diverse groups. These standards are available at the OMH website <www.omhrc.gov/CLAS>. In an attempt to articulate elements of clinical practice that define transcultural nursing, Leuning, Swiggum, Wiegert and McCullough-Zander (2002) outlined proposed standards of transcultural nursing practice. There are currently many other resources available to nursing and other health professions that address the issue of cultural competency and the provision of culturally competent care (Figure 1).
Figure 1.
| Transcultural Health Care URLs. |
|
A Model of Cultural Competence
The Process of Cultural Competence in the Delivery of Healthcare Services Model is a model of cultural competence that defines cultural competence as "the process in which the nurse continuously strives to achieve the ability and availability to effectively work within the cultural context of a client individual, family or community" (Campinha-Bacote,1998, p. 6). This process requires nurses to see themselves as becoming culturally competent, rather than being culturally competent. It includes consideration of cultural desire, cultural awareness, cultural knowledge, cultural skill (conducting culturally sensitive assessments) and cultural encounters (Campinha-Bacote, 2002a). This model of cultural competence is pictorially depicted as a volcano (Figure 2), which symbolically represents that it is cultural desire which stimulates the process of cultural competence. When cultural desire erupts, it gives forth the desire to enter into the process of becoming culturally competent by being humble to the process of seeking cultural awareness, by obtaining cultural knowledge, by genuinely seeking cultural encounters, and by conducting culturally-sensitive assessments (showing cultural skill). To fully understand this model, each construct will be defined and discussed with examples coming from the many faces of diversity.
| Figure 2. |
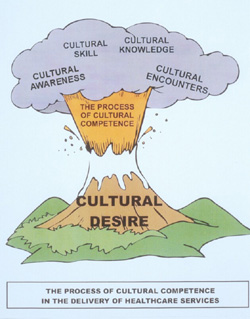 |
| Campinha-Bacote, Copyright 2002*; Reprinted with Permission by Transcultural C.A.R.E. Associates |
Cultural Desire
Cultural desire is defined as the motivation of the nurse to "want to" engage in the process of becoming culturally aware, culturally knowledgeable, culturally skillful, and seeking cultural encounters. It stands in contrast to the feeling of "having to" participate in this process (Campinha-Bacote, 1999). Cultural desire is the pivotal and key construct of cultural competence, for it is the nurse's desire that evokes the entire process of cultural competence. This desire must come from one's aspiration, and not out of one's desperation.
Cultural desire involves the concept of caring. It has been said that people don't care how much you know, until they first know how much you care (Campinha-Bacote, 1998). Cultural desire includes a genuine passion to be open and flexible with others, to accept differences and build on similarities, and to be willing to learn from others as cultural informants. This type of learning is a life-long process which has been referred to as cultural humility (Tervalon & Murray-Garcia, 1998).
Cultural desire also involves the commitment of the nurse to care for all clients, regardless of their cultural values, beliefs, customs, or practices (Campinha-Bacote, in press, a). This may be difficult when caring for challenging patients or patients who engage in behaviors that may be in direct moral conflict with the nurse (e.g., abortion, substance abuse, spouse abuse, sexual addiction). An example of such a situation might arise when a nurse is asked to care for an Arab patient whose political and/or religious beliefs are in direct contrast to his/her beliefs. In this case, too, commitment to the process of cultural desire requires the nurse to be available to care for patients, even when there may be a natural instinct to resign oneself from the nurse- patient interaction.
One suggestion is to see the patient as a unique human being.
We all come from the same race - the human race, with similar basic human needs. |
We all come from the same race - the human race, with similar basic human needs. Our goal in providing culturally responsive care is to find common ground. Berlin and Fowkes' (1982) LEARN Model can assist the nurse in this process. The mnemonic LEARN, represents the process of listening, explaining, acknowledging, recommending and negotiating. The nurse must first listen to the patient's perception of the problem. This listening must be done in a non-judgemental manner, using encouraging comments such as, "Tell me more." The second step is for the nurse to explain his/her perception of the problem. The next key step is for the nurse to acknowledge not only the differences between the two perceptions of the problem, but to acknowledge the similarities. In developing a culturally responsive approach to care, the nurse must recognize differences, but build upon the similarities. The fourth step is to make recommendations which involve the patient. Finally, the nurse is to negotiate a treatment plan, considering that it is beneficial to incorporate selected aspects of the patient's culture into the plan.
Cultural Awareness
Cultural awareness is the self-examination and in-depth exploration of one's own cultural background (Campinha-Bacote, 1999). This process involves the recognition of one's biases, prejudices, and assumptions about individuals who are different. Without being aware of the influence of one's own cultural values, there is risk that the nurse may engage in cultural imposition. Cultural imposition is the tendency to impose one's beliefs, values and patterns of behavior upon another culture (Leininger, 1978).
One example of a culturally diverse group for which the nurse may want to closely examine his/her biases and beliefs, is the group of patients with disabilities. "Disability rights advocates often criticize health professionals, citing erroneous assumptions and failure to understand the perspectives of disabled persons" (Treloar, 1999, p. 358). Treloar further states that many health care providers practice from an illness-based model of disability and are unaware of the shift toward looking at disability as a problem that exists within the environment rather than the person. Some nurses haves used the term physically-challenged to capture this contemporary shift. Treloar asserts that effective interactions with people affected by disability begin with a personal awareness of one's thoughts and feelings surrounding disability, and encourages the nurse to ask the following questions: "Do my actions support stigma, isolation, and devaluation of people with disabilities? Am I sensitive to cultural differences in response to and support of this population?" (p. 363).
Cultural Knowledge
Cultural knowledge is the process of seeking and obtaining a sound educational foundation about diverse cultural and ethnic groups (Campinha-Bacote 1998). Obtaining cultural knowledge about the patient's health-related beliefs and values involves understanding their world view. The patients' world views will explain how they interpret their illness and how it guides their thinking, doing, and being. For example, although deafness can be defined physiologically as a loss of hearing, the majority of deaf people define it culturally, not physiologically (Stebnicki & Coeling, 1999). They believe that the most important quality of deafness is not the lack of hearing, but rather participation in the Deaf culture that is based on the American Sign Language and that values pride in this culture. Knowing the cultural values of the Deaf can help these clients use their usual coping responses in the midst of illness.
Treatment efficacy is another issue to address in the process of obtaining cultural knowledge. This involves obtaining knowledge in such areas as ethnic pharmacology. Ethnic pharmacology is the study of variations in drug metabolism among ethnic groups. There are several factors that are involved in determining responses to a specific drug in ethnic groups. These factors include genetic, environmental, structural, and cultural variation in ethnic groups. For example, therapeutic ranges of lithium differs among ethnic groups. Lin, Poland, and Lesser (1986) reported that the therapeutic range of lithium for manic patients in Japan and Taiwan to be 0.4 - 0.8 mEq/L, as compared to 0.6 - 1/2 mEq/L for patients in the United States.
In seeking knowledge about specific cultural groups, Campinha-Bacote (1998) and Purnell (1998) identified four stages that a nurse goes through: unconscious incompetence,conscious incompetence, conscious competence and unconsciouscompetence. Unconscious incompetence is not being aware that one is lacking cultural knowledge. This nurse has no awareness that cultural differences exist between themselves and the patient. Conscious incompetence is the awareness that one is lacking knowledge about another culture. The nurse may have recognized this incompetence by attending workshops on cultural diversity, reading articles or books on the topic, or having direct cross-cultural experiences with patients from culturally diverse backgrounds. These nurses posses "the ‘know that’ knowledge, but not the ‘know how’ knowledge" (Campinha-Bacote, 1998). They know that culture plays an important role in nursing, but do not know how to effectively use this knowledge. Conscious competence is the intentional act of learning about the patient's culture, verifying generalizations and providing culturally responsive nursing interventions. Unconscious competence is the ability of the nurse to spontaneously provide culturally responsive care to patients from diverse cultural backgrounds. The timing of an unconsciously competent nurse appears to be "a natural" when observing their interacting with patients from diverse cultures (Campinha-Bacote, 1998).
In obtaining cultural knowledge, it is critical to remember the concept of intra-cultural variation - there is more variation within cultural groups than across cultural groups.
...there is more variation within cultural groups than across cultural groups. |
No individual is a stereotype of one's culture of origin, but rather a unique blend of the diversity found within each culture, a unique accumulation of life experiences, and the process of acculturation to other cultures. Therefore, the nurse must develop the skill to conduct a cultural assessment with each patient.
Cultural Skill
Cultural skill is the ability to collect relevant cultural data regarding the patient's presenting problem as well as accurately performing a culturally-based, physical assessment (Campinha-Bacote, 1999). Leininger (1978) defines a cultural assessment as a "systematic appraisal or examination of individuals, groups, and communities as to their cultural beliefs, values and practices to determine explicit needs and intervention practices within the context of the people being served (pp.85-86). Cultural skill is also required when performing a physical assessment on ethnically diverse clients. The nurse should know how a patient's physical, biological and physiological variations influence their ability to conduct an accurate and appropriate physical evaluation (Purnell, 1998).
The literature provides the nurse with several cultural assessment tools (Giger & Davidhizar, 1999; Kleinman, Eisenburg, & Good, 1978; Purnell, 1998). However, the nurse must remember that conducting a cultural assessment is more than selecting a tool and asking the patient questions listed on the tool. The nurse's approach must be done in a culturally sensitive manner. A situation in which the nurse would need to be very culturally sensitive might arise when the nurse is collecting data regarding the sexual orientation of a patient. In such a situation the nurse can avoid offending the patient by increasing his/her skill in addressing this question with all patients, by listening with interest, and by remaining non-judgmental regarding any responses given by the patient. The nurse may need to have many encounters with patients from this cultural group in order to formulate questions that are culturally sensitive.
Cultural Encounters
Cultural encounter is the process which encourages the nurse to directly engage in face-to-face interactions with patients from culturally diverse backgrounds (Campinha-Bacote, 1998).
Interacting with patients from diverse cultural groups will refine or modify one's existing beliefs about a cultural group and will prevent stereotyping. |
Interacting with patients from diverse cultural groups will refine or modify one's existing beliefs about a cultural group and will prevent stereotyping. However, the nurse must be cautious and recognize that interacting with only three or four members from a specific ethnic group does not make one an expert on the cultural group. It is possible that these three or four individuals may or may not truly represent the stated beliefs, values, and/or practices of their specific cultural group.
Cultural encounters also involve an assessment of the patient's linguistic needs. Using a formally trained medical interpreter is necessary to facilitate accurate communication during the encounters. The use of untrained interpreters, friends, or family members may pose a problem due to their lack of knowledge regarding medical terminology and disease entities. This situation is heightened when children are used as interpreters. One glaring example of the failure to used a formally trained interpreter comes from the author’s experience. The case involved an obstetrical nurse who needed to communicate to her patient that she was going to deliver a stillbirth. The nurse did not speak Spanish and used the patient's 6 year old daughter to interpret to the mother that the baby was dead.
Applying the Model
This model is useful in caring for all people, because in reality we all belong to the same race - the human race, with all the same basic needs. However, it is important to remember that these needs may be expressed differently, and that "quality health care services" may mean something different for each patient. In providing these culturally responsive services, the nurse may want to consider the following question: "In caring for this cultural group, have I "ASKED" myself the right questions?" The mnemonic "ASKED" represents questions regarding desire, awareness, knowledge, skill, and encounters, and is presented in Figure 3 (Campinha-Bacote, 2002b).
|
Cultural Competence: Have I "ASKED" Myself the Right Questions?
|
|
A warenes: Am I aware of my personal biases and prejudices towards cultural groups different than mine?
S kill: Do I have the skill to conduct a cultural assessment and perform a culturally-based physical assessment in a sensitive manner ?
K nowledge: Do I have knowledge of the patient's world view and the field of biocultural ecology?
E ncounters: How many face-to-face encounters have I had with patients from diverse cultural backgrounds?
D esire: What is my genuine desire to "want to be" culturally competent?
|
Copyright 2002 by J. Campinha-Bacote*
Summary
In summary, this article discusses the concept of cultural competence and presents The Process of Cultural Competence in the Delivery of Healthcare Services Model. Using this Model includes consideration of cultural desire, cultural awareness, cultural knowledge, cultural skill, and cultural encounters. The need to recognize that this Model is useful for all clients because we are all members of the same human race is emphasized. The mnemonic "ASKED" is provided to assist nurses in using this Model in their daily practice.
Author
Josepha Campinha-Bacote, PhD, APRN, BC, CTN, FAAN
e-mail: meddir@aol.com
Dr. Campinha-Bacote is the President and Founder of Transcultural C.A.R.E. Associates, a private consultation service which focuses on clinical, administrative, research, and educational issues in transcultural health care and mental health. She received her B.S. from the University of Rhode Island, her M.S. from Texas Women's University and her Ph.D from the University of Virginia. She is certified by the American Nurses Association as a Clinical Nurse Specialist in Psychiatric & Mental Health Nursing, and by the Transcultural Nurses Society as a Certified Specialist in Transcultural Nursing. Dr. Campinha-Bacote holds the academic titles of Adjunct Professor at several universities including The Ohio State University in Columbus, Ohio, and the University of Cincinnati, in Cincinnati, Ohio. In 2000, Dr. Campinha-Bacote served on the National Advisory Committee to the U.S. Department of Health and Human Services Office of Minority Health to develop standards for Culturally and Linguistically Appropriate Services (CLAS) in Healthcare. She currently serves as a consultant to the National Center For Cultural Competence (NCCC) in Washington, DC and to Health Resources and Services Administration (HRSA) Managed Care Technical Assistance Center of the U.S. Department of Health and Human Services.
Correction added May 2008 to reflect Copyright 2002 by J. Campinha-Bacote for Figures 2 and 3.
Article published January 31, 2003
References
Berlin, E., & Fowkes, W. (1982). A teaching framework for cross-cultural health care. The Western Journal of Medicine, 139(6), 934-938.
Campinha-Bacote, J. (in press). Cultural desire: The development of a spiritual construct of cultural competence. Journal of Christian Nursing.
Campinha-Bacote, J. (2002a). The process of cultural competence in the delivery of healthcare services: A model of care. Journal of Transcultural Nursing, 13(3), 181-184.
Campinha-Bacote, J. (2002b). Cultural competence in psychiatric nursing: Have you "ASKED" the right questions? Journal of the American Psychiatric Association, 8(16), 183-187.
Campinha-Bacote, J. (1999). A model and instrument for addressing cultural competence in health care. Journal of Nursing Education, 38(5), 203-207.
Campinha-Bacote, J. (1998). The process of cultural competence in the delivery healthcare services: A culturally competentm Model of care (3rd ed.). Cincinnati, OH: Transcultural C.A.R.E. Associates. (Available from www.transculturalcare.net)
Cross, T., Bazron, B., Dennis, K., & Isaacs, M. (1989). Towards a culturally competent system of care. Volume 1. Washington, DC: CASSP Technical Assistance Center.
Dolnick, E. (1993). Deafness as a culture. Atlantic, 272(3), 37-53.
Giger, J., & Davidhizar, R. (1999). Transcultural nursing. St. Louis: Mosby Year Book.
Harwood, A. (1981). Ethnicity and medical care. Boston: Harvard University Press.
Kleinman, A., Eisenburg, L., & Good, B. (1978). Culture, illness and care. Annals of Internal Medicine, 88, 251-258.
Kroeber, A., & Kluckhohn, C. (1978). Culture: A critical review of concepts and definitions. NY: Krauss Reprint Co. (Original work published in 1952).
Leininger, M. (1978). Transcultural nursing: Concepts, theories, research, & practice. NY: John Wiley & Sons.
Leuning, C., Swiggum, P., Wiegert, H. ,& McCullough-Zander, K. (2002). Proposed standards for transcultural nursing. Journal of Transcultural Nursing, 13(1), 40- 46.
Lin, K., Poland, R. Lesser, I. (1986). Ethnicity and psychopharmacology. Culture, Medicine, and Psychiatry, 10,151-165.
Purnell, L. (1998). Transcultural diversity and health care. In L. Purnell and B. Paulanka (Eds.), Transcultural health care: A culturally competent approach. Philadelphia: F.A. Davis.
Stebnicki, J., & Coeling, H. (1999). The culture of the deaf. Journal of Transcultural Nursing, 10(4), 350-357.
Tervalon, M., & Murray-Garcia, J. (1998). Cultural humility versus cultural competence: A critical distinction in defining physician training outcomes in multicultural education. Journal of Health Care for the Poor and Underserved, 9(2), 117-125.
Treloar, L. (1999). People with disabilities - the same, but different: Implications for health care practice. Journal of Transcultural Nursing, 10(4), 350-357.
Tylor, E. (1871). Primitive Culture. Volume 1. London: Bradbury, Evans and Co.
Correction added May 2008 to reflect Copyright 2002 by J. Campinha-Bacote for Figures 2 and 3.

