Between 2017 and 2060, the United States (US) will experience considerable growth in its older population. In 2060, the population aged 65 and over is projected to be 98 million, more than double its population of 46 million in 2016 (Population Reference Bureau, 2016). Additionally, the 65-and-older age group’s share of the total population will rise from 15 percent to nearly 24 percent (Population Reference Bureau, 2016). With this aging population, chronic diseases are inevitable and pose a great challenge to the healthcare system in the US. The most common, and costly chronic diseases and conditions are heart disease, stroke, cancer, type 2 diabetes, obesity, and arthritis (Centers for Disease Control and Prevention [CDC], 2017). In 2012 about 117 million people had one or more chronic health conditions; and this number accounted for about half of all adults (CDC, 2017). One in four adults had two or more chronic health conditions (CDC, 2017). In the US, about 80% of older adults have at least one chronic diseases, and 77% have at least two chronic diseases (National Council on Aging [NCOA], 2016). Almost two-thirds of all deaths in recent years resulted from heart disease, cancer, stroke, and diabetes (NCOA, 2016). For instance, 12.2 million Americans aged 60 and older are affected by diabetes (23% of the older population) and 90% of Americans aged 55+ are at risk for hypertension (NCOA, 2016). Also, seven of the top 10 causes of death in 2014 were chronic diseases, with heart disease and cancer together accounting for nearly 46% of all deaths (CDC, 2017).
Seventy five percent of the healthcare spending in the US is for chronic diseases (NCOA, 2016) and 86% of the nation’s $2.7 trillion annual healthcare expenditures are spent for people with chronic and mental health conditions together (CDC, 2017). For example, cardiovascular disease costs averaged $316.1 billion in 2012–2013 annually (CDC, 2017). This included the direct medical expenses cost, $189.7 billion plus the indirect costs of $126.4 billion related lost productivity (CDC, 2017). As a result of living longer, along with the added costs of attending to multiple chronic diseases and increases in the cost of daily living care, older individuals may not be able to provide care for themselves.
The high cost of long-term care is not covered by most insurance benefits (Reinhard, Levine, & Samis, 2012). Insurance generally does not cover long-term professional help. Only the expensive, long-term care insurance policies cover long-term care insurance; and the majority of Americans do not have this more expensive coverage. With this reality, family caregivers are essential to provide the complex care required for their loved ones.
Family caregivers in the home are essential for providing the care needed for family members who cannot care for themselves, so as to prevent their care receiver's institutionalization and consequently to decrease/avoid the cost of hospitalizations and emergency department (ED) visits (Reinhard et al., 2012). Providing support and professional instructions to family caregivers is crucial to address the family caregiver’s role on the healthcare team and for continuity of care (Reinhard et al., 2012). It is also important to improve family caregivers’ quality of life, both physically and mentally (Reinhard et al., 2012). The purpose of this column is to describe recent policy development related to family caregiving. Specifically, we will describe major findings and recommendations from the Home Alone: Family Caregivers Providing Complex Chronic Care report (Reinhard et al., 2012) and subsequent state and national efforts. We will conclude with recommendations for healthcare providers.
Family caregivers are involved in activities of daily living (ADLs) and instrumental activities of daily living (IADLs) for their loved ones (Reinhard et al., 2012). In addition, family caregivers are involved in complex, health-related activities that would ordinarily be called medical/nursing tasks and performed by healthcare providers (Reinhard et al., 2012). In the first, nationally representative, population-based online survey of 1,677 family caregivers, the caregivers managed numerous medical/nursing tasks in varying frequencies (Reinhard et al., 2012). Figure 1 summarizes these medical/nursing tasks provided by caregivers; for the full report and detailed results, see Home alone report.
Figure 1. Medical/Nursing Tasks Provided by Family Caregivers.
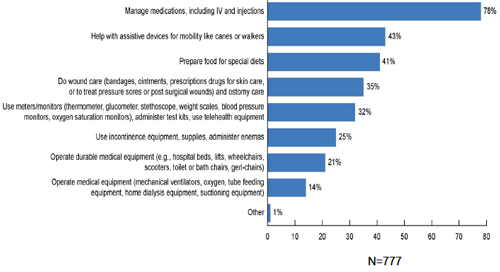
Reprinted with permission (Reinhard et al., 2012, p. 20).
Among 1,677 family caregivers who were surveyed in this study and who provided unpaid care to a relative or friend age 18 or older in the past 12 months, 46% performed medical/nursing tasks for their care recipient with multiple, chronic, physical and cognitive conditions (Reinhard et al., 2012). Among all these family caregivers, 69% reported not receiving home visits by healthcare professionals (Reinhard et al., 2012).
Seventy-eight percent of medical/nursing tasks involved medication management; half of the caregivers managed five to nine prescribed medications (Reinhard et al., 2012). This care, which is clearly complex, was performed in the past only by licensed professionals. Other frequently performed activities included help with assistive devices (43%), preparation of special diets (41%), and assistance with wound care 35% (Reinhard et al., 2012).
Other important findings in this report are related to family caregivers’ quality of life. The effects of providing medical/nursing tasks on family caregivers' quality of life included both positive and negative effects on their physical and mental health (Reinhard et al., 2012). For instance, positive effects were eased/less worry (44%) and feeling close (44%) (Reinhard et al., 2012). On the other hand, negative effects included employment/taking time off (14%), dealing with many suppliers/professionals (23%), and constantly worrying (32%) (Reinhard et al., 2012). Almost a third of caregivers reported fair or poor physical health (32%) and 40 % reported feeling down, depressed, or hopeless (Reinhard et al., 2012). Among family caregivers who provided five or more medical/nursing tasks, more than half reported feeling down, depressed or hopeless within the last two weeks, and 35% reported fair or poor health (Reinhard et al., 2012). Approximately half of the family caregivers who helped with medical/nursing tasks believed that they were providing care to avoid nursing home placement, and 43% believed they were allowing more independence (Reinhard et al., 2012). These findings illustrate the family caregivers’ vital role as part of the healthcare team (Reinhard et al., 2012). Findings from this survey provide compelling evidence that family caregiving is much more than assisting with personal care and household chores; rather it has evolved into non-professionals providing medical/nursing tasks (Reinhard et al., 2012).
This Home Alone report is an excellent example of research translation into policy and how research results are employed and adapted as policies and practical programs as shown in Figure 2. The Home Alone report offered 10 recommendations to guide the “coordinated efforts” to highlight the need for support and help for family caregivers (Reinhard et al., 2012). The main policy recommendations are Recommendations 7 and 8. Recommendation 7 notes that “Federal policymakers should proactively consider family caregivers in developing new models of care that focus on coordination and quality improvement,” while Recommendation 8 states that "policymakers should proactively consider family caregivers in funding and policy development” (Reinhard et al., 2012, p. 3). Those two recommendations are considered a call for action to support the family caregivers’ need for training and designed instructions (Reinhard et al., 2012). This report invites the state and federal government to develop new policies, funding resources, and care delivery systems to integrate family caregivers’ role as a healthcare team member.
Figure 2. Research Utilization Toolkit.

Reprinted with permission from Toolkits by K4Health (2016).
In the 5-year period following the publication of this report, 39 states and territories have enacted state law based on model state legislation, The Caregiver Advise, Record and Enable (CARE) Act (Reinhard & Ryan, 2017) as shown in Figure 3.
Figure 3: States with the CARE Act Enacted or under Consideration, July 2017.

Reprinted with permission from Reinhard and Ryan (2017).
The CARE Act focuses on family caregivers’ vital role and targets three key areas for policy change: a) caregivers’ visibility and integration in care from the admission throughout hospital stay; b) provision of adequate and clear messages regarding patient discharge and care timeline; and c) caregivers need for simple organized directions and care instructions (Reinhard & Ryan, 2017). For instance, the Ohio Caregiving Act, passed by Ohio General Assembly in March of 2017, acknowledges the rights of family caregivers (American Association of Retired Persons [AARP] Ohio, 2017). The Ohio Caregiving Act requires hospitals to: (a) designate a family caregiver in the patient’s medical record; (b) inform family care giver when patient is discharged; and (c) offer the family care giver instruction and demonstration of medical tasks they will be expected to provide at home for their loved ones (such as administer medications, dressing wounds and operating medical equipment) (AARP Ohio, 2017, p.3).
National efforts have been spearheaded by the Home Alone Alliance, a partnership of public, private, and non-profit agencies. Their goal is to serve as "a catalyst for change in the way health care organizations and professionals interface with family caregivers" (Reinhard & Ryan, 2017, p. 6). State and national efforts to address caregivers' needs have led to the introduction of a bill in the U.S. Congress.
The U.S. Senate Bill 1028, the RAISE Family Caregivers Act: Recognize, Assist, Include, Support, and Engage Family Caregivers Act, was introduced in May of 2017 (S.1028). S.B. 1028 is primarily a bill to establish and maintain a National Family Caregiving Strategy (S.1028). This bill is sponsored by Senator (Sen.) Susan Collins [R-ME], and originally co-sponsored by Sen. Tammy Baldwin, [D-WI], Sen. Lisa Murkowski [R-AK], and Sen. Michael F. Bennet [D-CO]. Later co-sponsors include: Sen. Debbie Stabenow [D-MI], Sen. Christopher A. Coons [D-DE], Sen. Joe Donnelly[D-IN], Sen. Al Franken [D-MN], Sen. Elizabeth Warren [D-MA], Sen. Amy Klobuchar [D-MN], Sen. Bill Nelson [D-FL], and Sen. Jeff Merkley [D-OR] (S.1028). This bill was referred to the Health, Education, Labor, and Pensions Senate Committee in May and was placed on the Senate Legislative Calendar under General Orders (S.1028). A hearing was held on June 14 at a Special Committee on Aging (S.1028). No further bill actions have been reported (S.1028).
SB 1028 directs the Department of Health and Human Services (DHHS) to “develop, maintain, and periodically update a National Family Caregiving Strategy and to identify specific actions that Federal, State and local government, communities, healthcare, long term services and supports and other providers, employers and others can take to recognize and support family caregivers to address their diverse needs” (S.1028, p. 2.). Additionally, it was noted that HHS shall assemble a Family Caregiving Advisory Council to guide in recognizing and identifying the needs and the required support for family caregivers (S.1028)
The Family Caregiving Advisory Council members will consist of Federal members and appointed members (S.1028). The appointed members in the Advisory council are not more than 15, not representative of federal agencies, and shall include:
At least one representative of each of the following: (a) family caregivers, (b) older adults with long-term services and supports needs, including older adults facing disparities,(c) individuals with disabilities, (d) advocates for family caregivers, older adults with long-term services and supports needs, and individuals with disabilities, (e) health care and social service providers, (f) long-term services and supports providers, (g) employers, (h) paraprofessional workers, (i) state and local officials, (j) accreditation bodies, (k) relevant industries, (l) veterans, and (m) as appropriate, other experts in family caregiving (S.1028, pp. 4-5).
The Federal members are nonvoting members and shall consist of the following: (a) the administrator of the Centers for Medicare & Medicaid Services (or the administrator's designee), the administrator of the Administration for Community Living (or the administrator's designee who has experience in both aging and disability), (c) the Assistant Secretary for the Administration for Children and Families (or the Assistant Secretary's designee),(d) the Secretary of Veterans Affairs (or the Secretary's designee),(e) the Secretary of Labor (or the Secretary's designee), (f) the Secretary of the Treasury (or the Secretary's designee), (g) the National Coordinator for Health Information Technology (or the National Coordinator's designee), (h) the Administrator of the Small Business Administration (or the Administrator's designee), (i) the Chief Executive Officer of the Corporation for National and Community Service (or the Chief Executive Officer's designee), and (j) the heads of other Federal departments or agencies (or their designees), as appointed by the Secretary or the Chair of the Advisory Council (S.1028, p.5).
This bill also recommends that the Advisory Council members be sought to reflect the diversity of family caregivers in order to provide the essential services and supports (S.1028).
Nurses have a responsibility to promote this national effort. Nurses and nursing leadership should contribute to the development of this national strategy. Nurses could fit under multiple categories of the Advisory Council. There should be at least one nurse on the Advisory Council. We, as nurses, have a unique perspective that is critical to the conversation and subsequent development of a national strategy for caregivers.
The expected role from you as a reader and a professional is to be a part of this public implementation policy advocating for family caregivers’ rights. Your role may include the following activities:
- Remain aware and updated regarding your state legislation regarding the CARE Act to provide the required support for family caregivers. If your state does not have legislation, work with your state nurses association, legislators and other groups to introduce legislation. Be part of state efforts.
- Reach out to your national legislators and discuss SB 1028 the RAISE Family Caregivers Act and CARE Act requesting their support. Be part of national efforts.
- Organize an open day in local hospitals and other healthcare settings to shed light on the family care providers’ role in supporting the RAISE Family Caregivers Act and CARE Act. This open day could be part of a massive statewide public education campaign.
- Facilitate social media initiatives (Facebook, Twitter) to increase the public awareness and/or support about this act including a family caregivers Facebook page to share the universality of the issue.
- Invite your local legislators to caregivers’ homes to meet with the family members and family caregivers in-order-to understand their experiences and discuss obstacles faced when providing care.
- Be a part of caregiver advocacy and support organizations, such as local AARP and National Alliance for Caregiving, to support their new changes in practice that are required to unify the effort toward one optimal goal.
- Involve nursing organizations as part of these state and national efforts, and support AARP and other members of the Home Alone Alliance.
- Show appreciation to your legislators who support the CARE Act and the RAISE Family Caregivers Act to continue their efforts working on passing the proposed bill.
In summary, almost no one will be immune in their lifetime to the necessity to care for a loved one at home. Each of us must become involved at the state and national level so that state and national caregiving strategies reflect nursing values and input is adopted.
Greer Glazer, RN, CNP, PhD, FAAN
Email: glazergr@UCMAIL.uc.edu
Abeer Alhaj Ali, RN, BSN, MSN
Email: alhajaaa@mail.uc.edu
